Fill out healthcare billing forms
with AI.
Healthcare billing forms are the essential communication link between medical providers, insurance carriers, and government health programs. These documents serve as the foundation for reimbursement, ensuring that medical services are accurately documented and that claims are processed according to specific regulatory standards. Without the correct submission of these forms, healthcare facilities can face significant delays in revenue cycles, leading to administrative bottlenecks and potential disruptions in patient care services.
By continuing, you acknowledge Instafill's Privacy Policy and agree to get occasional product update and promotional emails.
About healthcare billing forms
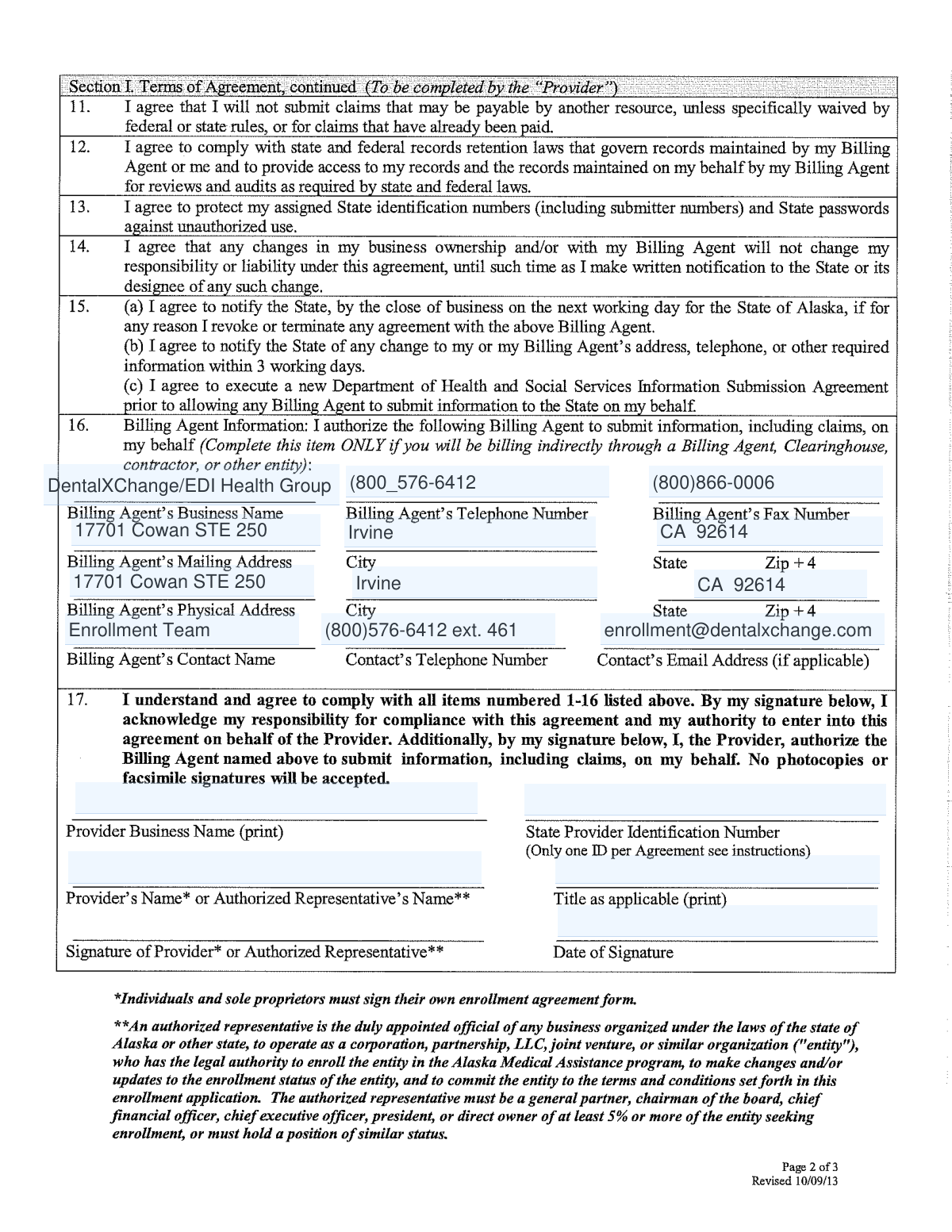
Medical administrators, billing specialists, and independent practitioners typically utilize these forms during critical transitions, such as enrolling in electronic data interchange (EDI) systems or updating provider credentials. For instance, forms like the Medicaid of Alaska Provider Electronic Remittance (835) Authorization are vital for practices moving away from manual paper processes toward more efficient electronic claims. Whether you are managing a private practice or a large hospital network, accurately completing these forms is a prerequisite for maintaining compliance and securing timely payments from various payers.
Manually entering repetitive provider data, National Provider Identifiers (NPI), and tax information into complex PDFs can be a tedious and error-prone process. Tools like Instafill.ai use AI to fill these healthcare billing forms in under 30 seconds, ensuring that sensitive data is handled accurately and securely. This practical approach allows administrative teams to streamline their workflows and focus more on practice management rather than manual data entry.
Forms in This Category
- Enterprise-grade security & data encryption
- 99%+ accuracy powered by AI
- 1,000+ forms from all industries
- Complete forms in under 60 seconds
How to Choose the Right Form
Navigating healthcare billing can be complex, especially when coordinating with state-specific Medicaid programs. This category focuses on the essential paperwork required for providers operating within the state of Alaska who wish to modernize their billing cycle and ensure consistent cash flow through electronic systems.
Managing Alaska Medicaid Electronic Claims
If you are a healthcare provider seeking to transition from manual to electronic billing with Alaska Medicaid, the primary document you need is the Medicaid of Alaska Provider Electronic Remittance (835) Authorization and Claims Enrollment Form.
This form serves as the gateway for providers to interact with Electronic Data Systems (EDS). You should choose this form if you are looking to perform any of the following actions:
- New Enrollments: For providers setting up electronic claims submission for the first time.
- Modifications: For existing providers who need to update their electronic billing details, change their address, or switch clearinghouses.
- Cancellations: If you need to officially terminate your electronic remittance agreement with the state.
Key Requirements for Successful Completion
To ensure your application is processed without delays by the Alaska Department of Health, have the following information ready before you start filling out the form on Instafill.ai:
- Provider Identification: You will need your legal business name, physical address, and National Provider Identifier (NPI).
- Tax Information: Ensure you have your Federal Tax Identification Number (TIN) or Employer Identification Number (EIN) available.
- Authorized Signatory: The form requires a signature from an individual with the legal authority to enter into agreements on behalf of the healthcare entity.
Why This Form is Essential
By completing the Medicaid of Alaska Provider Electronic Remittance (835) Authorization and Claims Enrollment Form, you gain access to the 835 transaction set. This allows your practice to receive Electronic Remittance Advice (ERA), which automates the posting of payments and adjustments to your practice management system, significantly reducing administrative overhead and manual entry errors. Using Instafill.ai ensures that your submission is legible, professional, and completed accurately the first time.
Form Comparison
| Form | Purpose | Who Files It | Frequency | Key Requirements |
|---|---|---|---|---|
| Medicaid of Alaska Provider Electronic Remittance (835) Authorization and Claims Enrollment Form | Enables healthcare providers to submit electronic claims and receive digital remittance advice from Alaska Medicaid. | Healthcare providers or billing entities seeking electronic status with Alaska Medicaid through EDS. | Submitted during initial enrollment or when modifying/canceling existing electronic billing arrangements. | Requires legal provider name, TIN/EIN, National Provider Identifier (NPI), and an authorized signature. |
Tips for healthcare billing forms
Ensure your NPI and Federal Tax Identification Number (TIN) exactly match your official registry records. Inconsistent identifiers are the most common cause of processing delays or rejected electronic enrollment requests.
AI-powered tools like Instafill.ai can complete these complex healthcare billing forms in under 30 seconds with high accuracy. This is a significant time-saver for busy practices, and your sensitive provider data remains completely secure throughout the automated filling process.
Only an authorized representative of the healthcare provider should sign these enrollment forms to ensure legal compliance. Submissions with unauthorized signatures will be returned, requiring you to start the entire application process over.
If you are enrolling for Electronic Remittance Advice (835), double-check that your billing software is compatible with the state's specific data format. This ensures that once the form is processed, your system can automatically reconcile payments without manual entry.
Always save a copy of the completed and signed enrollment form before submitting it to the payer. Having a digital record allows you to quickly reference your submission if there are questions regarding your electronic billing status during a future audit.
Submit a new enrollment or modification form immediately if your practice changes its physical address, legal name, or banking details. Failing to update these forms can lead to interrupted payments or remittance data being sent to the wrong location.
Frequently Asked Questions
Healthcare billing forms are used to facilitate the reimbursement process between medical providers and insurance entities or government programs. They ensure that services rendered are accurately documented and that the provider receives the correct payment for those services through standardized data exchange.
These forms are primarily used by healthcare providers, medical billing offices, and administrative staff at facilities that provide services covered by insurance. They are necessary for any professional or entity that needs to establish a payment relationship with a payer like Medicaid or a private insurer.
Standard claim forms are used to request payment for specific medical services, while electronic remittance forms focus on setting up the infrastructure for digital communication. Enrollment forms allow providers to receive automated payment details and electronic advice rather than waiting for paper statements.
Most provider forms require the legal name of the practice, physical and mailing addresses, and tax identifiers such as an EIN or TIN. Additionally, professional identifiers like the National Provider Identifier (NPI) are essential for verifying the provider's identity and credentials.
The NPI is a unique 10-digit identification number used to identify healthcare providers in standard transactions across the industry. It is a mandatory requirement for most billing and enrollment forms to ensure that payments are correctly attributed to the licensed professional or facility.
Depending on the specific form, they are typically submitted to state Medicaid offices, private insurance carriers, or third-party clearinghouses. Many organizations now prefer or require these forms to be uploaded through secure online portals or submitted via encrypted electronic channels.
Yes, healthcare billing forms can be filled out using AI tools like Instafill.ai. These tools can accurately extract data from your source documents and place it into the correct fields in under 30 seconds, significantly reducing the risk of manual entry errors.
While manual entry can take quite some time, using an AI-powered service allows you to complete these forms in under 30 seconds. This efficiency helps medical administrative staff manage high volumes of paperwork without sacrificing accuracy.
If a provider's business details change, they usually need to submit a modification or update form to the relevant payer or agency. This ensures that payments and remittance advice continue to reach the correct legal entity and location without administrative delays.
While some small practices may still use paper-based systems, most large payers and government programs like Medicaid strongly encourage or mandate electronic billing processes. Electronic enrollment helps reduce processing times and minimizes the risk of lost or delayed paperwork.
Glossary
- 835 Transaction
- The standard electronic format used by health plans to provide explanation of payment and remittance information to healthcare providers.
- Electronic Remittance Advice (ERA)
- A digital version of a medical insurance payment explanation that details how a claim was processed, including adjustments and final payment amounts.
- NPI (National Provider Identifier)
- A unique 10-digit identification number issued to healthcare providers in the United States to standardize electronic health transactions.
- TIN/EIN
- A nine-digit Tax Identification Number or Employer Identification Number assigned by the IRS to identify a business entity for tax and billing purposes.
- EDI (Electronic Data Interchange)
- The automated, computer-to-computer exchange of standard business documents, such as claims and remittances, between healthcare providers and payers.
- Clearinghouse
- A third-party service that acts as an intermediary, checking medical claims for errors and formatting them correctly before sending them to insurance payers.
- Adjudication
- The legal and administrative process used by health insurance companies to determine their financial responsibility for a submitted medical claim.
- Provider Enrollment
- The administrative process of applying to a health insurance plan's network so a healthcare professional can receive direct reimbursement for services.