Fill out Indiana Medicaid forms
with AI.
Indiana Medicaid forms are essential documents for managing healthcare within the state's public insurance system. These forms, ranging from enrollment applications to specific clinical requests, ensure that residents receive the medical assistance they need while maintaining compliance with state regulations. For healthcare providers and patients alike, these documents act as the bridge between needing care and securing the financial coverage required to pay for it, making them a cornerstone of the Indiana Health Coverage Programs (IHCP).
By continuing, you acknowledge Instafill's Privacy Policy and agree to get occasional product update and promotional emails.
About Indiana Medicaid forms
Typically, these forms are utilized by medical offices, hospitals, and social workers who need to coordinate benefits for their patients. A common example is the Prior Authorization Request Form, which providers must submit to verify that a specific procedure or piece of equipment is medically necessary before treatment begins. Navigating these insurance authorization forms is a standard part of managing health coverage, ensuring that approvals are processed correctly to avoid claim denials or unexpected out-of-pocket expenses for the patient.
Completing these detailed healthcare forms can be time-consuming and prone to manual errors. Tools like Instafill.ai use AI to fill these forms in under 30 seconds, handling sensitive data accurately and securely. By automating the data entry process, healthcare professionals can focus more on patient care and less on the administrative burden of paperwork.
Forms in This Category
| Form Name | Pages | |
|---|---|---|
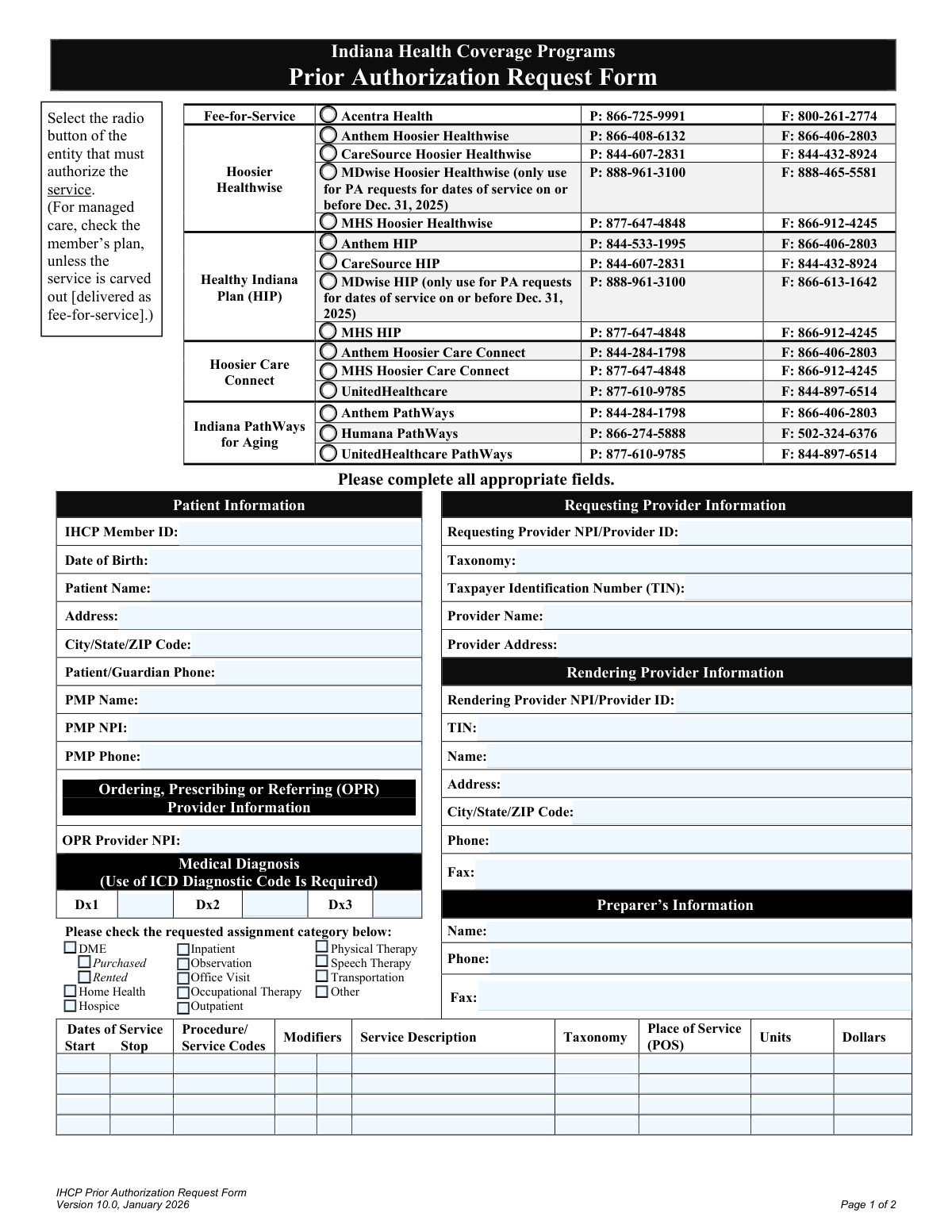
| 1. | Indiana Health Coverage Programs Prior Authorization Request Form | 2 |
- Enterprise-grade security & data encryption
- 99%+ accuracy powered by AI
- 1,000+ forms from all industries
- Complete forms in under 60 seconds
How to Choose the Right Form
Navigating the requirements for Indiana Medicaid, specifically under the Indiana Health Coverage Programs (IHCP), often comes down to ensuring that medical services are pre-approved to avoid claim denials and unexpected costs. While the documentation process can be complex, the forms in this category are designed to streamline communication between healthcare providers and the state’s insurance plans.
For Medical Service Pre-Approval
If you are a healthcare provider or an administrative staff member seeking approval for a patient's upcoming treatment, the Indiana Health Coverage Programs Prior Authorization Request Form is the primary document you will need. This form is the standard tool used across various IHCP delivery systems to request coverage for:
- Specialized medical procedures and surgeries
- Durable medical equipment (DME) and supplies
- Specific outpatient services that require a clinical necessity review
- Non-emergency services that fall outside standard coverage limits
Determining Your Filing Needs
Before you begin filling out the form, ensure your situation meets the following criteria to ensure you are using the right paperwork:
- Provider Initiation: This form is typically completed by the rendering or ordering provider, rather than the patient, as it requires clinical justification.
- Program Alignment: Confirm that the patient is currently enrolled in an IHCP-managed plan, such as Traditional Medicaid, Hoosier Healthwise, or the Healthy Indiana Plan (HIP).
- Supporting Documentation: The Indiana Health Coverage Programs Prior Authorization Request Form must be accompanied by clinical notes or a physician's order to prove medical necessity.
Using AI to Streamline IHCP Filing
Manual data entry into medical forms can lead to clerical errors that delay patient care. By utilizing the Indiana Health Coverage Programs Prior Authorization Request Form on Instafill.ai, you can leverage AI to ensure all required fields are populated accurately. Our platform can also take non-fillable PDF versions of these state forms and convert them into interactive documents, allowing your office to submit requests faster and maintain organized digital records.
Form Comparison
| Form | Purpose | Who Files It | When to Use |
|---|---|---|---|
| Indiana Health Coverage Programs Prior Authorization Request Form | Request pre-approval for medical services, procedures, or equipment to ensure insurance coverage. | Healthcare providers on behalf of Indiana Health Coverage Programs (IHCP) members. | Before rendering specific medical services or providing equipment to confirm medical necessity. |
Tips for Indiana Medicaid forms
Ensure that the member’s IHCP identification number and date of birth exactly match their Medicaid card. Even a single digit error can lead to an immediate rejection or a 'member not found' status, causing unnecessary delays in patient care.
Prior authorization forms often require supporting documentation, such as clinical notes or diagnostic results, to prove medical necessity. Always double-check that your attachments are relevant and clearly labeled to help the reviewer make a quick and informed determination.
Incomplete provider information is a common reason for processing delays in Indiana Medicaid forms. Make sure to include the correct National Provider Identifier (NPI) and the specific taxonomy code associated with the service being requested to ensure the form is routed to the correct department.
When managing multiple Indiana Medicaid forms, using AI-powered tools like Instafill.ai can be a significant time-saver. These tools can complete complex forms in under 30 seconds with high accuracy while ensuring your data stays secure throughout the process.
Only mark a request as 'Urgent' if a delay would seriously jeopardize the member's life or health. Misusing the urgent status for routine procedures can lead to administrative bottlenecks and may require additional justification from the provider.
Keep a copy of every submitted prior authorization form and the accompanying confirmation number. Having an organized digital record allows you to quickly reference previous requests if you need to file an appeal or provide additional information at a later date.
Verify that all procedure codes (CPT) and supply codes (HCPCS) are the most recent versions accepted by Indiana Medicaid. Using outdated or incorrect codes can result in an automatic denial, requiring you to restart the entire authorization process from scratch.
Frequently Asked Questions
Indiana Medicaid forms, specifically those under the Indiana Health Coverage Programs (IHCP), are used to manage benefits, request services, and document medical necessity. These forms ensure that healthcare providers and members comply with state regulations to receive reimbursement for medical services and equipment.
Typically, the healthcare provider or the facility requesting the service is responsible for completing and submitting the Prior Authorization (PA) form. While the patient is the beneficiary, the provider must supply the clinical documentation and medical justification required by the IHCP to prove the service is necessary.
These forms must be submitted and approved before the requested medical service, procedure, or equipment is provided to the patient. Failing to obtain authorization in advance can result in the insurance plan denying payment, which may lead to unexpected costs for the patient or the provider.
These forms are used for members enrolled in Indiana Health Coverage Programs, including Traditional Medicaid, Hoosier Healthwise, the Healthy Indiana Plan (HIP), and Hoosier Care Connect. Depending on the member's plan, the form is submitted either to a Managed Care Entity like Anthem or MHS, or to Gainwell Technologies.
Yes, you can use AI tools like Instafill.ai to complete Indiana Medicaid forms quickly and accurately. The AI can extract data from your source documents and place it into the correct fields on the form in under 30 seconds, significantly reducing the risk of manual entry errors.
While traditional manual entry can take 15 to 20 minutes per form, using an AI-powered service like Instafill.ai allows you to complete the process in under 30 seconds. The tool automates the data extraction and placement, making the workflow much more efficient for busy medical offices.
You will generally need the member's Medicaid ID number, provider information including NPI and taxonomy codes, and specific procedure or HCPCS codes. Additionally, the form requires clinical justification, and providers often need to attach supporting documentation such as lab results or clinical notes.
Submission instructions vary based on the member's specific program. Forms are typically faxed or uploaded through a secure online portal to the appropriate Managed Care Entity or to the state's fiscal agent for Traditional Medicaid members.
If a form is incomplete or lacks sufficient clinical evidence, it may be returned to the provider for correction or denied entirely. Using digital tools to ensure all required fields are accurately filled can help prevent these administrative delays and ensure patients receive timely care.
Yes, many official Indiana Medicaid forms are distributed as static PDFs that do not allow for easy typing. AI services like Instafill.ai can convert these non-fillable documents into interactive, fillable forms, allowing for a completely digital and streamlined submission process.
Providers should consult the IHCP Fee Schedule or the specific Managed Care Entity’s provider manual to check if a service code requires prior authorization. These requirements are updated periodically based on state policy changes and medical necessity guidelines.
Glossary
- IHCP (Indiana Health Coverage Programs)
- The umbrella program managed by the state of Indiana that includes Medicaid, the Healthy Indiana Plan (HIP), and Hoosier Healthwise.
- Prior Authorization (PA)
- A formal approval process where a healthcare provider must prove a treatment is necessary before Indiana Medicaid will agree to pay for it.
- RID (Recipient Identification Number)
- A unique 12-digit number assigned to an Indiana Medicaid member used to identify their specific coverage and eligibility status on forms.
- Medically Necessary
- A clinical standard used to decide if a service or supply is required to diagnose or treat an illness or injury according to established medical practice.
- NPI (National Provider Identifier)
- A unique 10-digit identification number assigned to healthcare providers and facilities used for billing and authorization purposes.
- CPT/HCPCS Codes
- Standardized numeric or alphanumeric codes used on forms to identify specific medical procedures, services, or equipment being requested.
- FSSA (Family and Social Services Administration)
- The Indiana state agency that oversees the administration of Medicaid and other social service programs.
- Retroactive Authorization
- A request for coverage of medical services that have already been provided, usually granted only in emergency situations or specific administrative delays.