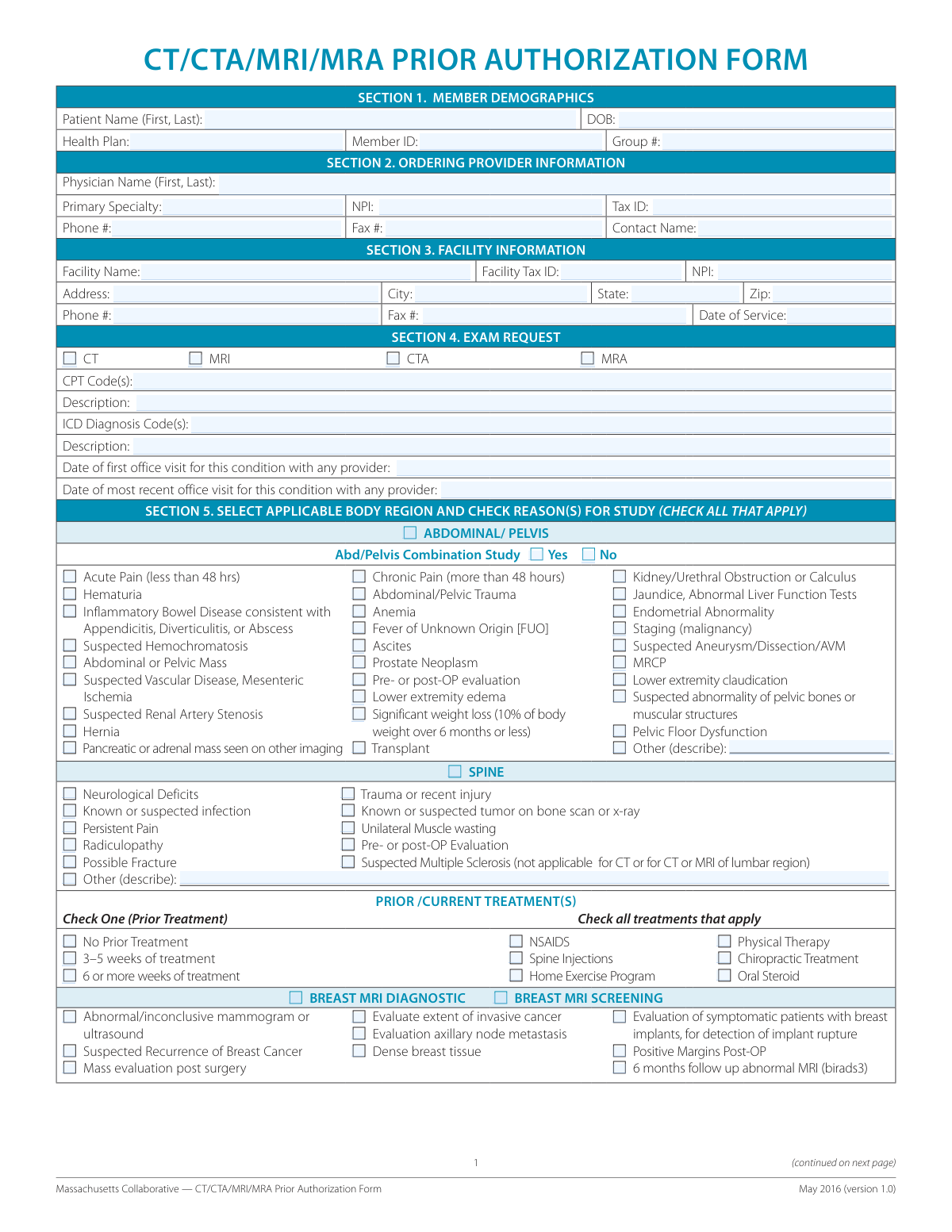
Fill out insurance approval forms
with AI.
Insurance approval forms, often referred to as prior authorization or pre-certification requests, are essential documents used to confirm that a proposed medical service or treatment meets the specific coverage criteria of a health plan. These forms serve as a critical bridge between healthcare providers and insurance carriers, ensuring that complex procedures or high-cost medications are medically necessary before they are performed. Navigating this process correctly is vital for preventing unexpected out-of-pocket costs for patients and minimizing the administrative burden of denied claims for medical practices.
By continuing, you acknowledge Instafill's Privacy Policy and agree to get occasional product update and promotional emails.
About insurance approval forms
Typically, medical office administrators, nurses, and billing specialists are responsible for managing these forms. They are frequently required for advanced diagnostic imaging, such as CT scans and MRIs, as well as for specialized surgical procedures or long-term therapies. Because each insurance provider has unique requirements, completing these documents accurately is often time-consuming but necessary to maintain a smooth workflow within a clinical setting.
Handling these documents manually often leads to clerical errors or delays in patient care. Tools like Instafill.ai use AI to fill these forms in under 30 seconds, ensuring data is handled accurately and securely while streamlining the entire authorization process. By automating the data entry for complex documents like the Massachusetts Collaborative Prior Authorization form, providers can focus more on patient outcomes rather than repetitive administrative paperwork.
Forms in This Category
| Form Name | Pages | |
|---|---|---|
| 1. | Massachusetts Collaborative — CT/CTA/MRI/MRA Prior Authorization Form | 2 |
- Enterprise-grade security & data encryption
- 99%+ accuracy powered by AI
- 1,000+ forms from all industries
- Complete forms in under 60 seconds
How to Choose the Right Form
Navigating the insurance approval process is critical for ensuring that medical procedures are covered and that patients aren't left with unexpected bills. While this category focuses on insurance approval forms, the specific documentation you need depends heavily on the type of procedure, the insurance carrier, and your geographic location.
Advanced Imaging in Massachusetts
If you are a healthcare provider or a patient in Massachusetts preparing for a high-tech diagnostic scan, the Massachusetts Collaborative — CT/CTA/MRI/MRA Prior Authorization Form is the primary document you will encounter. This form is a standardized tool used across the state to streamline requests for advanced imaging.
This form is specifically designed for:
- CT and CTA Scans: Computed Tomography and Computed Tomography Angiography.
- MRI and MRA Scans: Magnetic Resonance Imaging and Magnetic Resonance Angiography.
When to Use This Form
You should choose this specific form if your situation meets the following criteria:
- Location: The patient is receiving care or the provider is practicing within the state of Massachusetts.
- Medical Necessity: You need to provide detailed clinical evidence to a health plan to justify the need for advanced imaging before the scan is performed.
- Standardization: This is a collaborative form, meaning it is accepted by many different health plans across the state, reducing the need for multiple different carrier-specific forms.
Tips for a Successful Submission
Insurance companies often deny claims due to missing clinical data or incorrect coding. When filling out the Massachusetts Collaborative Prior Authorization Form, ensure you have the following ready:
- The specific CPT codes for the imaging requested.
- The patient’s relevant medical history and previous treatments (such as physical therapy or medication) that did not resolve the issue.
- The ordering physician’s NPI and contact information.
Using Instafill.ai allows you to take this complex document and complete it with AI assistance. This reduces manual entry errors and speeds up the submission process, helping patients get their diagnostic scans scheduled and approved faster.
Form Comparison
| Form | Primary Purpose | Services Covered | Geographic Scope |
|---|---|---|---|
| Massachusetts Collaborative — CT/CTA/MRI/MRA Prior Authorization Form | Requesting prior authorization to ensure insurance coverage for advanced imaging. | Advanced imaging studies including CT, CTA, MRI, and MRA scans. | Specifically for healthcare providers and insurance plans within Massachusetts. |
Tips for insurance approval forms
Errors in diagnostic or procedure codes are the most common reason for immediate insurance denial. Ensure the codes entered on your form match the physician's clinical notes and the specific imaging study being requested.
Most insurance carriers require recent clinical notes or previous test results to prove medical necessity for advanced imaging. Having these digital documents ready to reference while filling out your form prevents unnecessary delays and back-and-forth with the insurer.
AI-powered tools like Instafill.ai can complete these complex insurance forms in under 30 seconds with high accuracy. Your data stays secure during the process, providing a practical and reliable way to handle high volumes of paperwork without manual entry errors.
A single digit error in a patient's insurance ID can cause a form to be rejected before it even reaches a medical reviewer. Always verify the current member ID and group number directly from the patient’s most recent insurance card to ensure a match.
Insurance companies operate on strict timelines for reviewing prior authorizations. Note the date of submission and any confirmation numbers so you can efficiently follow up if a response is not received within the expected timeframe.
Ensure you are using the correct version of the form for the specific imaging study, such as differentiating between an MRI and a CT scan. Using a specialized collaborative form when required ensures that you provide all the specific data points the insurer needs for that category.
Frequently Asked Questions
Insurance approval forms, often called prior authorization or pre-certification forms, are documents used by healthcare providers to request coverage for specific treatments or diagnostic tests before they occur. These forms help insurance companies verify that a procedure is medically necessary and falls within the patient's plan benefits.
Advanced imaging studies like CT scans and MRIs are high-cost procedures that insurance companies monitor closely. Requiring a prior authorization form ensures that the clinical evidence supports the need for the scan, helping to manage healthcare costs and prevent unnecessary radiation exposure.
The healthcare provider’s office or the facility where the procedure will take place usually completes and submits these forms. While the patient may need to provide some personal insurance details, the clinical justification must be documented by a medical professional.
Yes, AI tools like Instafill.ai can be used to fill out insurance approval forms in under 30 seconds. The technology accurately extracts clinical data and patient information from source documents and places it directly into the required fields of the PDF.
These forms should be submitted as soon as the physician determines the procedure is necessary, ideally several days or weeks before the scheduled appointment. Submitting early allows enough time for the insurance company to review the clinical notes and issue an approval number.
If a procedure requiring prior authorization is performed without an approved form on file, the insurance company may deny the claim entirely. This often results in the patient being held responsible for the full cost of the service or the provider having to write off the charges.
Filling out these detailed forms manually can take 15 to 20 minutes, but using an AI-powered service like Instafill.ai reduces this time to less than 30 seconds. The AI automates the data entry process, ensuring high accuracy while saving significant administrative time for medical staff.
Most insurance approval forms require recent office visit notes, results from previous conservative treatments, and any relevant laboratory or diagnostic test results. This documentation provides the medical necessity evidence required for the insurance company to grant approval.
While some regions use standardized documents like the Massachusetts Collaborative form, many insurance carriers have their own proprietary forms. It is important to check the specific requirements of the patient's health plan to ensure the correct document is utilized.
Once a form is submitted, providers usually receive a confirmation number or can check the status via the insurance company's online provider portal. If a decision isn't reached within the expected timeframe, the medical office typically follows up by phone to check for any missing information.
Glossary
- Prior Authorization
- A process where a healthcare provider must get approval from a health insurance plan before a specific service or procedure is performed for it to be covered.
- Medical Necessity
- The standard used by insurance companies to decide if a treatment or test is essential and appropriate for a patient’s specific medical condition based on clinical evidence.
- CPT Code
- A standardized five-digit code used to identify the specific medical service or diagnostic procedure being requested for approval.
- ICD-10 Code
- An international system of alphanumeric codes used by doctors to classify and code all diagnoses, symptoms, and procedures.
- NPI Number
- A unique 10-digit identification number assigned to healthcare providers that must be included on all insurance administrative and financial transactions.
- Rendering Provider
- The medical professional or facility that will actually perform the diagnostic test or treatment once the insurance company grants approval.
- Requesting Provider
- The physician or specialist who orders the medical service and initiates the insurance approval process on behalf of the patient.
- Clinical Documentation
- The medical records, such as office notes and lab results, that provide the necessary evidence to support the request for a procedure.