Fill out Massachusetts health insurance forms
with AI.
Navigating the healthcare system in Massachusetts requires precise documentation to ensure that patients receive the care they need while maintaining insurance coverage. This category of forms covers the essential paperwork required by state health plans and providers to coordinate medical services, verify eligibility, and secure necessary approvals. From routine administrative updates to complex clinical requests, these documents serve as the vital link between medical necessity and financial reimbursement.
By continuing, you acknowledge Instafill's Privacy Policy and agree to get occasional product update and promotional emails.
About Massachusetts health insurance forms
Healthcare providers, clinic administrators, and patients typically interact with these forms during critical stages of care. For example, when a physician orders advanced diagnostic imaging like an MRI or CT scan, specific prior authorization forms must be submitted to demonstrate that the procedure meets clinical guidelines. Accurate completion is essential to avoid claim denials and ensure that treatment is not delayed by administrative hurdles. Whether you are managing a single patient’s request or a high volume of clinic paperwork, these forms are central to the Massachusetts healthcare experience.
Completing detailed medical documentation can be a time-intensive process that distracts from patient care. Tools like Instafill.ai use AI to fill these forms in under 30 seconds, handling sensitive data accurately and securely to streamline your workflow. This technology simplifies the transition from static PDF documents to completed filings, allowing you to focus on health outcomes rather than paperwork.
Forms in This Category
| Form Name | Pages | |
|---|---|---|
| 1. | Massachusetts Collaborative — CT/CTA/MRI/MRA Prior Authorization Form | 2 |
- Enterprise-grade security & data encryption
- 99%+ accuracy powered by AI
- 1,000+ forms from all industries
- Complete forms in under 60 seconds
How to Choose the Right Form
Navigating the administrative requirements of the Massachusetts healthcare system is essential for ensuring that patients receive timely care without unexpected financial burdens. If you are a healthcare provider or medical administrative professional in the Commonwealth, selecting the correct documentation for medical necessity is the first step in a successful prior authorization process.
For Advanced Imaging and Radiology Requests
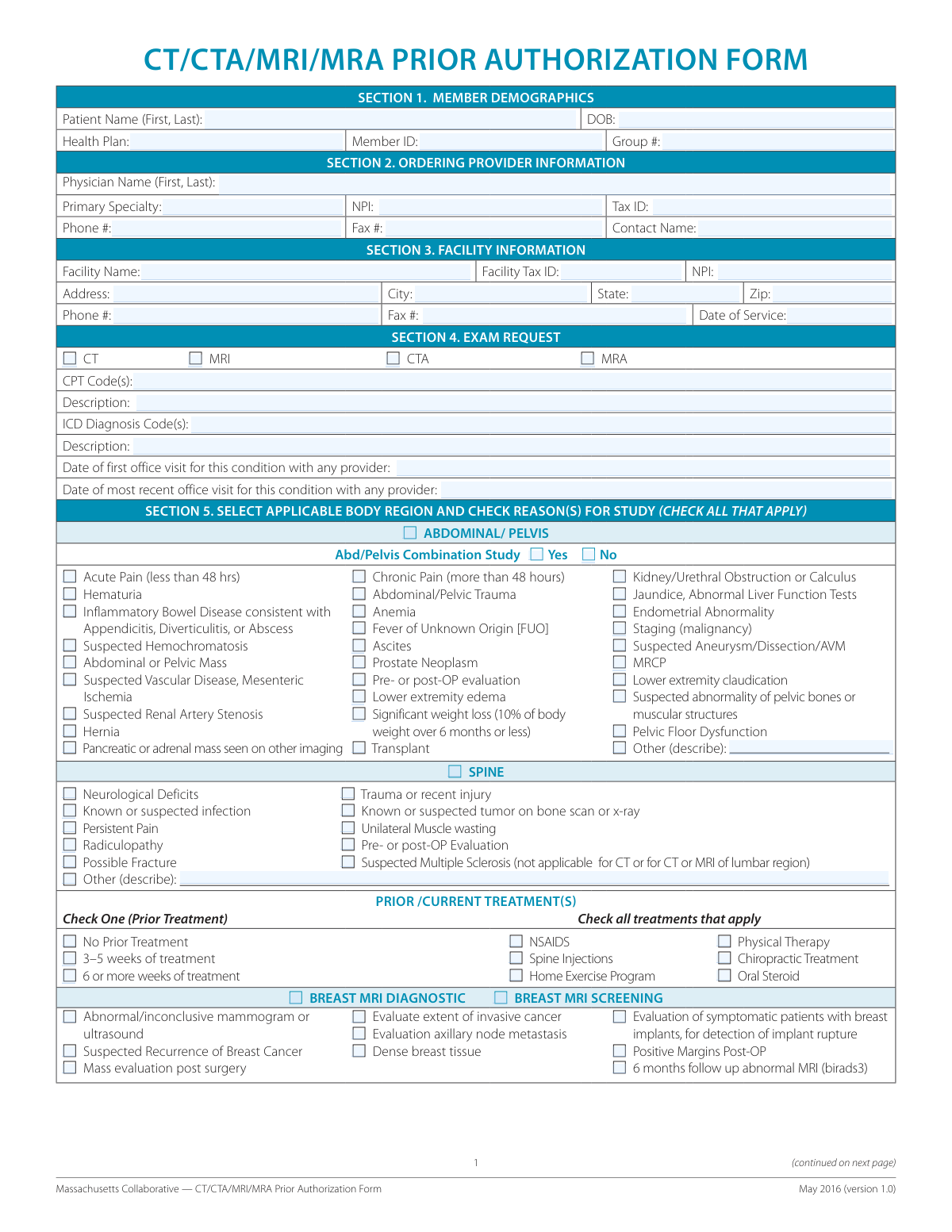
If your patient requires a high-tech imaging study, the Massachusetts Collaborative — CT/CTA/MRI/MRA Prior Authorization Form is the standard, unified document used across the state. This form is specifically designed to handle requests for:
- CT and CTA Scans: Computed tomography and angiography requests.
- MRI and MRA Scans: Magnetic resonance imaging and angiography requests.
This form is the correct choice when you need to demonstrate medical necessity to a health plan before a procedure takes place. Because it is a collaborative form, it is recognized by multiple insurers throughout Massachusetts, helping to streamline the approval process and reduce the need for plan-specific paperwork.
Who Should Use This Form?
This document is primarily intended for use by referring physicians and their clinical staff. It requires detailed clinical information, including previous treatments, relevant laboratory results, and the specific diagnostic questions being addressed by the requested scan.
Avoiding Claim Denials
To avoid claim denials or delays in patient care, ensure that all clinical justifications are accurately reflected on the Massachusetts Collaborative — CT/CTA/MRI/MRA Prior Authorization Form. Because these documents require significant detail, using an AI-powered tool like Instafill.ai can help you quickly populate provider information and patient data, ensuring the form is legible and complete before submission. This reduces the risk of administrative errors that could lead to billing issues or the need for a peer-to-peer review.
Form Comparison
| Form | Primary Purpose | Who Files It | Applicable Procedures |
|---|---|---|---|
| Massachusetts Collaborative — CT/CTA/MRI/MRA Prior Authorization Form | Requesting insurance approval for advanced medical imaging to ensure coverage. | Healthcare providers or medical office staff on behalf of patients. | Prior to conducting CT, CTA, MRI, or MRA diagnostic scans. |
Tips for Massachusetts health insurance forms
Ensure you have the patient's relevant medical history, previous test results, and physical exam notes ready before filling out the form. Attaching these supporting documents is essential for proving medical necessity and avoiding immediate denials or requests for more information.
Accurate coding is the backbone of Massachusetts prior authorization forms. Double-check that the procedure codes (CPT) match the requested imaging and that the diagnosis codes (ICD-10) clearly support the clinical need for the scan.
Missing or incorrect National Provider Identifier (NPI) numbers or Tax IDs can lead to immediate administrative rejections. Always confirm that both the ordering physician's and the rendering facility's identification numbers are current and accurate.
Managing complex medical forms can be time-consuming, but AI-powered tools like Instafill.ai can complete these forms in under 30 seconds with high accuracy. Your sensitive data stays secure during the process, making it a reliable way to handle high volumes of authorizations efficiently.
Only mark a request as 'urgent' if a delay would seriously jeopardize the patient's life or health. Misusing the urgent status can lead to administrative friction with Massachusetts health plans, so use the designation strictly according to clinical guidelines.
It is a common mistake to submit a perfectly filled form that lacks a final signature or the date of the request. Review the entire document to ensure all required fields are populated to prevent the form from being returned as incomplete or invalid.
Frequently Asked Questions
These forms are primarily used by healthcare providers to request approval from an insurance company before performing specific medical services. They help verify that a proposed diagnostic test or treatment is medically necessary and covered under the patient's specific health plan.
Generally, the ordering physician or their administrative staff is responsible for filling out and submitting these forms to the insurance carrier. While patients provide their insurance details, the medical justification and clinical history must be documented by the healthcare professional.
Advanced imaging studies such as CT scans, MRIs, CTAs, and MRAs frequently require prior authorization. Other specialized treatments, elective surgeries, or high-cost medications may also necessitate similar documentation to ensure reimbursement.
Submitting these forms in advance ensures that the insurance company will cover the costs of the procedure according to the patient's policy. Failing to obtain prior authorization can lead to claim denials, resulting in significant out-of-pocket costs for the patient.
These forms usually require patient demographics, insurance ID numbers, and specific CPT codes for the procedure. Additionally, providers must include clinical documentation, such as previous treatments or symptoms, to justify the medical necessity of the scan.
You should check the back of the patient's insurance card for the specific contact information or portal address for prior authorizations. Many Massachusetts plans use collaborative forms that are accepted by multiple major insurers across the state to streamline the process.
Yes, you can fill out Massachusetts health insurance forms using AI-powered tools. Services like Instafill.ai can accurately extract data from clinical notes or source documents and place it directly into the required PDF fields.
Using AI tools, you can fill these forms in under 30 seconds by automating the data entry process. This significantly reduces the administrative burden on medical staff and helps ensure that all fields are completed accurately to avoid processing delays.
If a request is denied, the provider can often file an appeal or request a peer-to-peer review with the insurance company's medical director. It is essential to review the specific denial reason and provide any additional clinical documentation that may have been missing from the initial submission.
While many insurers in Massachusetts use the Massachusetts Collaborative forms for consistency, some private plans or specialized networks may have their own unique requirements. It is best to verify the preferred form with the specific insurance carrier's provider portal before submission.
Glossary
- Prior Authorization (PA)
- A requirement by health insurance plans for patients or providers to obtain approval before a specific medical service or procedure is performed to ensure it will be covered.
- Medical Necessity
- A standard used by insurers to determine if a clinical service is essential, appropriate, and reasonable for the diagnosis or treatment of a patient's condition.
- Massachusetts Collaborative
- A group of health plans and provider organizations in Massachusetts that work together to create standardized forms and processes for the local healthcare industry.
- CPT Code
- A five-digit Current Procedural Terminology code used to identify the specific medical, surgical, or diagnostic service being requested for the patient.
- ICD-10 Code
- An international system of alphanumeric codes used by healthcare providers to classify and code all diagnoses, symptoms, and procedures.
- MRA (Magnetic Resonance Angiography)
- A specialized MRI scan that focuses specifically on the body's blood vessels to look for abnormalities like blockages or aneurysms.
- CTA (Computed Tomography Angiography)
- An imaging test that combines a CT scan with an injection of special dye to produce detailed pictures of blood vessels and tissues.
- Clinical Justification
- The medical documentation and reasoning provided by a physician to explain why a specific high-tech imaging test is the most appropriate next step for a patient.