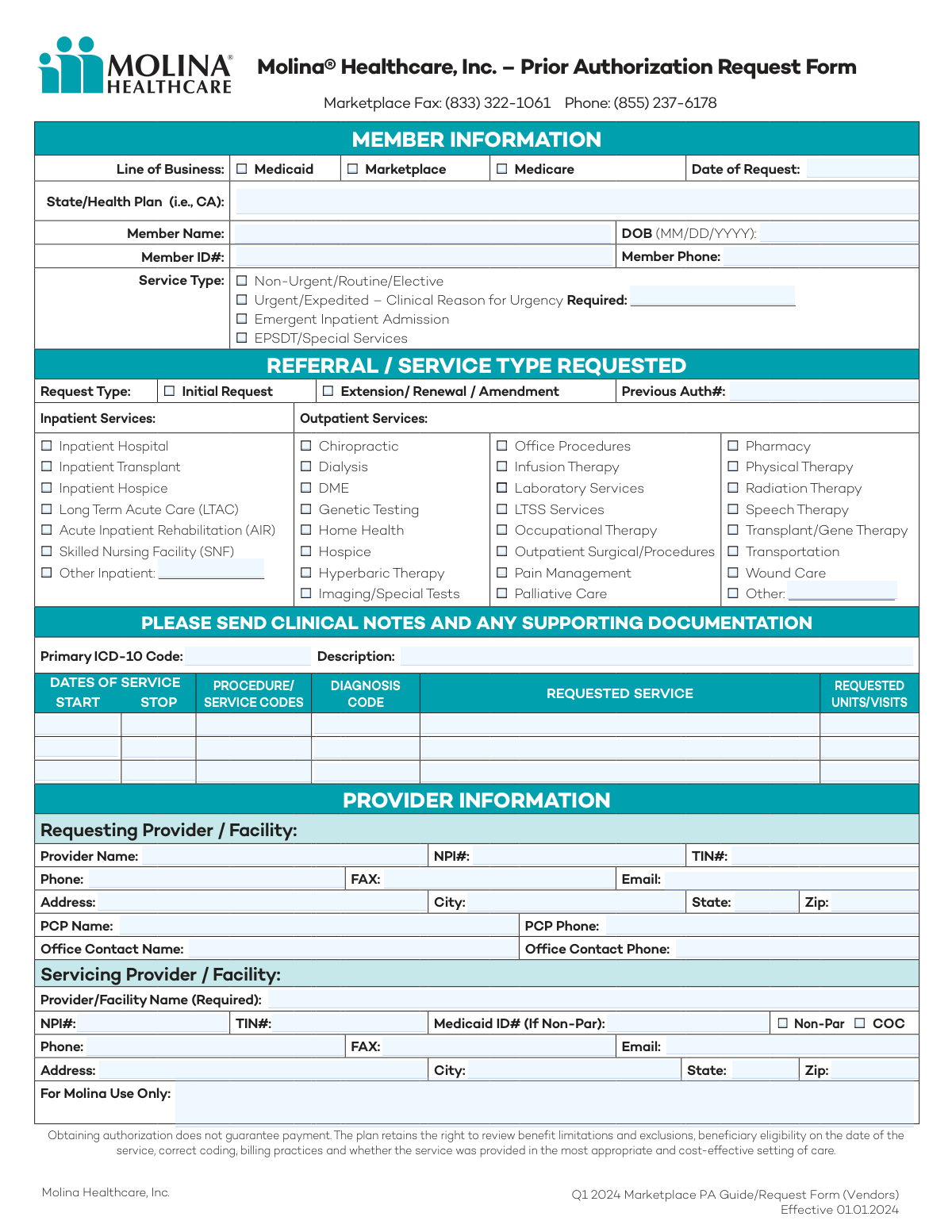
Fill out Molina Healthcare forms
with AI.
Molina Healthcare forms are essential for managing health coverage, particularly within Medicaid and Medicare plans. These documents facilitate communication between patients, healthcare providers, and the insurance carrier to ensure that medical services are properly authorized and reimbursed. Whether you are dealing with prior authorizations or general medical requests, having the correct documentation is vital for maintaining continuity of care and avoiding unexpected financial liabilities.
By continuing, you acknowledge Instafill's Privacy Policy and agree to get occasional product update and promotional emails.
About Molina Healthcare forms
Healthcare providers, clinic administrators, and patients often need these forms to secure approval for specific treatments, medications, or specialist visits. For example, a Prior Authorization Request Form is frequently used to confirm that a proposed medical procedure meets the insurer's criteria for medical necessity before the service is performed. Navigating these requirements accurately is critical for both the provider's billing process and the patient's access to timely healthcare. This ensures that the insurance plan covers the costs as expected, preventing administrative delays or denials.
Manually entering data into these complex medical documents can be time-consuming and prone to clerical errors. Tools like Instafill.ai use AI to fill these forms in under 30 seconds, handling sensitive data accurately and securely to streamline the administrative process. This allows medical staff and members to spend less time on paperwork and more time focusing on patient care and health outcomes.
Forms in This Category
| Form Name | Pages | |
|---|---|---|
| 1. | Molina Healthcare Prior Authorization Request Form | 2 |
- Enterprise-grade security & data encryption
- 99%+ accuracy powered by AI
- 1,000+ forms from all industries
- Complete forms in under 60 seconds
How to Choose the Right Form
Understanding Molina Healthcare Requests
Navigating insurance paperwork can be complex, especially when seeking approval for specialized medical care. If you are looking for Molina Healthcare forms, the primary document currently available is the Molina Healthcare Prior Authorization Request Form. This form is central to managing coverage and ensuring that medical services are approved before they occur.
When to Use the Prior Authorization Request Form
This form is the essential tool for healthcare providers and patients who need to confirm that a specific treatment will be covered by insurance before the service is provided. You should choose this form if:
- You are a Healthcare Provider: You need to submit a formal request for medical services, procedures, or specific medications to ensure they meet Molina’s medical necessity criteria.
- You are a Patient: You are coordinating with your doctor to secure approval for a surgery, specialist visit, or high-cost prescription to avoid unexpected out-of-pocket expenses.
- Preventing Denials: You want to avoid billing issues or claim denials by securing an authorization number prior to the date of service.
Why Prior Authorization is Essential
The Molina Healthcare Prior Authorization Request Form acts as a safeguard. By submitting this document, you ensure that the planned medical intervention aligns with the patient's insurance plan benefits. Without an approved authorization, Molina Healthcare may refuse to pay for the services, leaving either the provider or the patient responsible for the full cost. Using this form correctly is the first step in ensuring a smooth medical and billing experience.
Streamlining Your Submission
Filling out medical request forms manually often leads to errors that cause delays in care. Using Instafill.ai, you can quickly complete the Molina Healthcare Prior Authorization Request Form with AI assistance. Our platform can also take non-fillable PDF versions of these insurance forms and convert them into interactive documents, making it easier to submit accurate data to Molina Healthcare the first time.
Form Comparison
| Form | Purpose | Who Files It | When to Use | Key Requirements |
|---|---|---|---|---|
| Molina Healthcare Prior Authorization Request Form | Requesting approval for medical services or medications before treatment occurs | Healthcare providers or authorized clinical staff on behalf of patients | Before providing non-emergency services, procedures, or specific prescription medications | Patient ID, diagnosis codes, procedure details, and supporting clinical documentation |
Tips for Molina Healthcare forms
Ensure the patient’s Molina Healthcare ID number and date of birth match their insurance card exactly. Incorrect member details are a leading cause of administrative denials and can significantly delay the approval of urgent medical care.
Prior authorization requests often require supporting medical records, such as recent lab results or physician progress notes, to prove medical necessity. Including these documents with your initial submission prevents the insurer from needing to request more information later.
Double-check that all diagnostic and procedure codes are current and specific to the requested service. Using accurate codes helps the reviewer understand the exact nature of the request and reduces the likelihood of a coding-related rejection.
AI-powered tools like Instafill.ai can complete these complex forms in under 30 seconds with high accuracy. This technology automates data entry while ensuring your sensitive medical information stays secure during the process.
Keep a digital copy of every submitted form along with the date of submission and the confirmation receipt. Having this organized record is essential if you need to follow up on the status of a request or file an appeal.
Ensure the requesting and rendering provider information, including National Provider Identifier (NPI) numbers and Tax IDs, is accurate. Mismatched provider data can cause the authorization to be invalidated when the final medical claim is processed.
Frequently Asked Questions
Molina Healthcare forms are essential documents used by patients and healthcare providers to manage insurance benefits, request medical services, and update member information. These forms facilitate communication between the provider and the insurance company to ensure that medical care is correctly authorized and covered under a member's specific plan.
While these forms concern a patient's care, they are usually completed and submitted by the healthcare provider, such as a primary care physician or specialist. The provider must supply clinical justifications and medical codes to prove the necessity of the requested service or medication.
Prior authorization is a process used to verify that a proposed treatment, procedure, or medication is medically necessary and appropriate for the patient's condition. This step helps prevent unexpected billing issues by confirming that the service is covered by the insurance plan before the patient receives care.
Submission methods vary by state and plan but typically include secure provider portals, faxing to a specific department, or mailing the documents to a designated Molina Healthcare office. You should check the instructions at the bottom of the specific form or the Molina website for the correct contact information.
Yes, you can use AI tools like Instafill.ai to complete these forms quickly and accurately. The AI can extract data from your source documents and automatically place it into the correct fields on the Molina Healthcare form, even if the original PDF is not a fillable version.
Using AI-powered services like Instafill.ai, you can fill out complex medical forms in under 30 seconds. This process automates data entry and ensures that information is transcribed accurately from your records, significantly reducing the manual effort required.
Most medical request forms require the member's ID number, provider contact information, and specific medical codes like ICD-10 for diagnoses and CPT for procedures. Often, you must also attach supporting clinical documentation, such as lab results or previous treatment history, to support the request.
While deadlines can vary depending on the type of service, it is generally best to submit prior authorization forms as soon as the need for treatment is identified. Submitting well in advance of the scheduled service date helps avoid delays in care and ensures administrative processing is complete before the appointment.
If a request is denied, Molina Healthcare will provide a written explanation for the decision and outline the steps for an appeal. Providers can often resolve these issues by submitting additional medical records or participating in a peer-to-peer review with a medical director.
Yes, because insurance regulations and plan types differ across the country, Molina Healthcare often provides state-specific versions of their forms. It is important to select the form that corresponds to the member's location and specific plan type, such as Medicaid, Medicare, or Marketplace coverage.
Glossary
- Prior Authorization (PA)
- A requirement that your healthcare provider obtains approval from Molina Healthcare before performing certain services or prescribing specific medications to ensure coverage.
- Medically Necessary
- Healthcare services or supplies needed to prevent, diagnose, or treat an illness, injury, or its symptoms and that meet accepted standards of medicine.
- CPT Code
- Current Procedural Terminology codes are five-digit numbers used to identify the specific medical services and procedures being requested for approval.
- ICD-10 Code
- A standardized system of diagnosis codes used by healthcare providers to classify and report diseases, symptoms, and abnormal findings on medical forms.
- NPI (National Provider Identifier)
- A unique 10-digit identification number issued to healthcare providers in the United States, used on forms to identify the requesting or performing clinician.
- HCPCS Code
- Healthcare Common Procedure Coding System codes used to identify medical equipment, supplies, and services not covered by standard CPT codes.
- Expedited Request
- A fast-track authorization request used when a standard review timeframe could seriously jeopardize a patient's life, health, or ability to regain maximum function.
- TIN (Tax Identification Number)
- A unique nine-digit number used by the IRS to identify the healthcare provider's business or practice for billing and reporting purposes.