Fill out medication authorization forms
with AI.
Medication authorization forms, often referred to as prior authorization requests, are essential documents in the healthcare and insurance landscape. These forms serve as a formal bridge between healthcare providers and insurance companies, ensuring that patients can access specific prescription drugs that may not be on a standard formulary. By providing clinical justification and medical history, these forms help verify that a prescribed treatment is medically necessary and appropriate for the patient's condition.
By continuing, you acknowledge Instafill's Privacy Policy and agree to get occasional product update and promotional emails.
About medication authorization forms
Typically, healthcare providers, office administrators, and patients need these forms when an insurer requires pre-approval before covering a medication. This is common for high-cost drugs, medications with specific safety concerns, or when a physician believes a non-preferred drug is the best option for a patient who hasn't responded to standard treatments. Whether you are dealing with a Cigna Medication Prior Authorization Form or a general request for coverage, the goal is to document previous treatment attempts and diagnoses to prevent delays in care.
Completing these documents manually can be time-consuming for busy medical offices and stressful for patients waiting on treatment. Tools like Instafill.ai use AI to fill these forms in under 30 seconds, handling sensitive data accurately and securely to streamline the approval process. This allows providers to focus more on patient care rather than administrative paperwork.
Forms in This Category
| Form Name | Pages | |
|---|---|---|
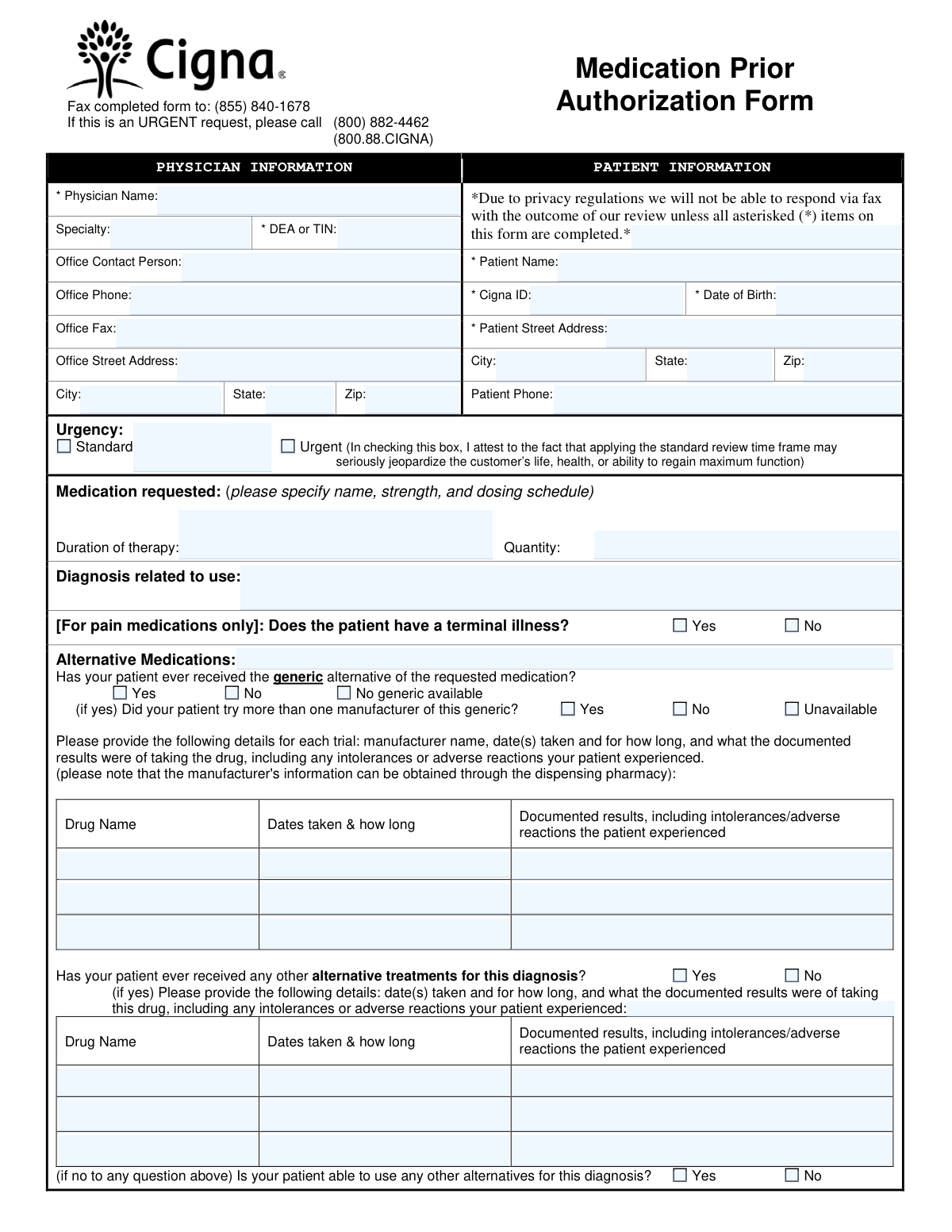
| 1. | Cigna Medication Prior Authorization Form | 2 |
| 2. | Medication Prior Authorization Request Form | 2 |
- Enterprise-grade security & data encryption
- 99%+ accuracy powered by AI
- 1,000+ forms from all industries
- Complete forms in under 60 seconds
How to Choose the Right Form
Selecting the correct medication authorization form is essential for ensuring patients receive their prescribed treatments without unnecessary delays. These forms serve as a formal bridge between healthcare providers and insurance companies, justifying the medical necessity of specific drugs.
Identify the Insurance Provider
The most important factor in choosing a form is the patient's insurance carrier. Using a carrier-specific form often speeds up the approval process because it contains the exact fields and codes required by that company's review team.
- For Cigna Policyholders: Use the Cigna Medication Prior Authorization Form. This document is tailored specifically for Cigna’s internal review criteria. It is designed to help physicians document medical necessity and list previous treatment attempts (step therapy) that align with Cigna’s specific formulary requirements.
- For Other or General Insurers: If you are dealing with a different provider or a smaller regional insurer that does not provide a proprietary document, the Medication Prior Authorization Request Form serves as a standard template. This generic version includes all the fundamental sections required by most insurers, such as diagnosis codes, clinical justification, and patient medical history.
Consider the Clinical Justification
Regardless of which form you choose, ensure you have the following information ready to input into Instafill.ai to ensure a successful submission:
- Patient Information: Full name, policy ID number, and date of birth.
- Provider Details: National Provider Identifier (NPI) and contact information for follow-ups.
- Medication Specifics: The exact drug name, dosage, and frequency being requested.
- Supporting Evidence: Documentation of why the "preferred" drugs on the insurer's list were ineffective or are contraindicated for the patient.
By selecting the Cigna Medication Prior Authorization Form for Cigna-specific claims or the Medication Prior Authorization Request Form for general clinical justifications, you can streamline your administrative workflow and focus more on patient care.
Form Comparison
| Form | Primary Purpose | Insurance Provider | Key Requirements |
|---|---|---|---|
| Cigna Medication Prior Authorization Form | Request pre-approval for non-preferred drugs under Cigna insurance plans. | Specific to Cigna health insurance members and their providers. | Medical necessity, diagnosis codes, and history of previous treatments. |
| Medication Prior Authorization Request Form | Generic request for medication coverage from various insurance carriers. | Universal; applicable to most standard health insurance companies. | Clinical justification, patient medical history, and alternative medication failure. |
Tips for medication authorization forms
Clearly state the diagnosis and explain why the requested medication is medically necessary for the patient. Including specific ICD-10 codes and clinical evidence helps insurance reviewers understand the urgency and appropriateness of the treatment.
Many insurers require 'step therapy,' meaning the patient must try preferred drugs first. List any medications the patient has already tried, including the dosages and reasons for failure, such as adverse reactions or lack of efficacy.
Completing multiple authorization requests manually is time-consuming and prone to errors. AI-powered tools like Instafill.ai can complete these forms in under 30 seconds with high accuracy while ensuring your sensitive data stays secure during the process.
Ensure the patient’s insurance ID number, group number, and date of birth are perfectly accurate. Even a minor typo in the member information can lead to an immediate administrative denial, delaying the patient's access to medication.
Supporting documentation like recent lab work or clinical progress notes can significantly strengthen your case. Providing this information upfront prevents insurance companies from sending 'request for information' letters that pause the approval clock.
Only mark a request as 'expedited' or 'urgent' if the standard turnaround time would seriously jeopardize the patient's health. Overusing the urgent status for routine refills can lead to increased scrutiny from the insurer's pharmacy benefit manager.
Always save a copy of the completed form and any confirmation receipts for your medical records. This documentation is essential if you need to follow up on a pending status or file an appeal after an initial denial.
Frequently Asked Questions
These forms are used by healthcare providers to request that an insurance company cover the cost of a specific prescription drug. This process is typically required when a medication is expensive, not on the insurer's standard list of preferred drugs, or requires clinical oversight for safety reasons.
While a patient or administrative assistant can fill out basic contact information, the clinical sections must be completed by a licensed healthcare provider. The prescribing physician must provide the medical justification, diagnosis codes, and treatment history necessary for the insurance company to make a decision.
The correct form depends on the patient's insurance provider and the specific plan they are enrolled in. For example, if the patient has coverage through Cigna, you should use their specific carrier form; otherwise, a general prior authorization request form is often used for other insurers.
Most forms require the patient's insurance ID number, the provider's National Provider Identifier (NPI), and specific ICD-10 diagnosis codes. You will also need to provide the drug name, dosage, and documentation of any other medications the patient has already tried for the condition.
Yes, AI tools like Instafill.ai can fill out these forms in under 30 seconds by accurately extracting and placing data from source documents or medical records. This helps medical offices reduce manual entry errors and ensures that complex clinical information is mapped to the correct fields.
Completing these forms manually can be time-consuming, but using an online AI service allows you to finish the process in less than half a minute. These platforms can also turn non-fillable PDF versions into interactive documents, making it easier to type directly into the form.
Once the form is filled out and signed by the healthcare provider, it is usually faxed or submitted through a secure online portal to the insurance company's pharmacy benefit management department. The specific submission instructions and fax numbers are typically listed on the form itself.
If an insurer denies the request, they will send a notification explaining the reason, such as a lack of medical necessity or a requirement to try a different drug first. In these cases, the healthcare provider can choose to file an appeal or submit additional clinical documentation to support the request.
While most insurance carriers use standardized forms nationwide, some states have specific laws requiring the use of a universal state-mandated prior authorization form. It is important to verify if your state requires a specific version before submitting the request to the insurer.
Processing times vary by insurer and the urgency of the medical condition, but most companies provide a response within two to five business days. Urgent requests can often be expedited if the healthcare provider indicates that a delay could seriously jeopardize the patient's health.
Glossary
- Prior Authorization (PA)
- A requirement from a health insurance company that a healthcare provider must obtain approval before a specific medication will be covered. This process confirms that the treatment is medically necessary and meets the insurer's coverage guidelines.
- Formulary
- A continually updated list of prescription drugs covered by a specific health insurance plan. If a medication is 'non-formulary,' an authorization form is typically required to request coverage for that drug.
- Medical Necessity
- The clinical standard used by insurers to determine if a treatment or medication is essential for a patient's health condition. Authorization forms require providers to prove medical necessity through diagnoses and clinical data.
- Step Therapy
- An insurance policy requiring a patient to try one or more lower-cost medications before 'stepping up' to a more expensive drug. Authorization forms often ask for documentation of which previous treatments failed.
- ICD-10 Code
- A standardized alphanumeric code used by healthcare providers to classify and identify specific diseases and medical conditions. These codes are mandatory on authorization forms to justify the use of a specific medication.
- NPI (National Provider Identifier)
- A unique 10-digit identification number assigned to healthcare providers in the United States. It is a required field on medication forms to identify the prescribing physician for processing and billing.
- Quantity Limit
- A restriction on the amount of a specific medication an insurance company will cover over a set period. Authorization forms may be submitted to request an exception to these limits based on a patient's unique needs.
- Clinical Justification
- The detailed medical evidence provided by a physician to explain why a specific drug is required. This often includes lab results, a history of allergic reactions to alternatives, or the specific stage of a disease.