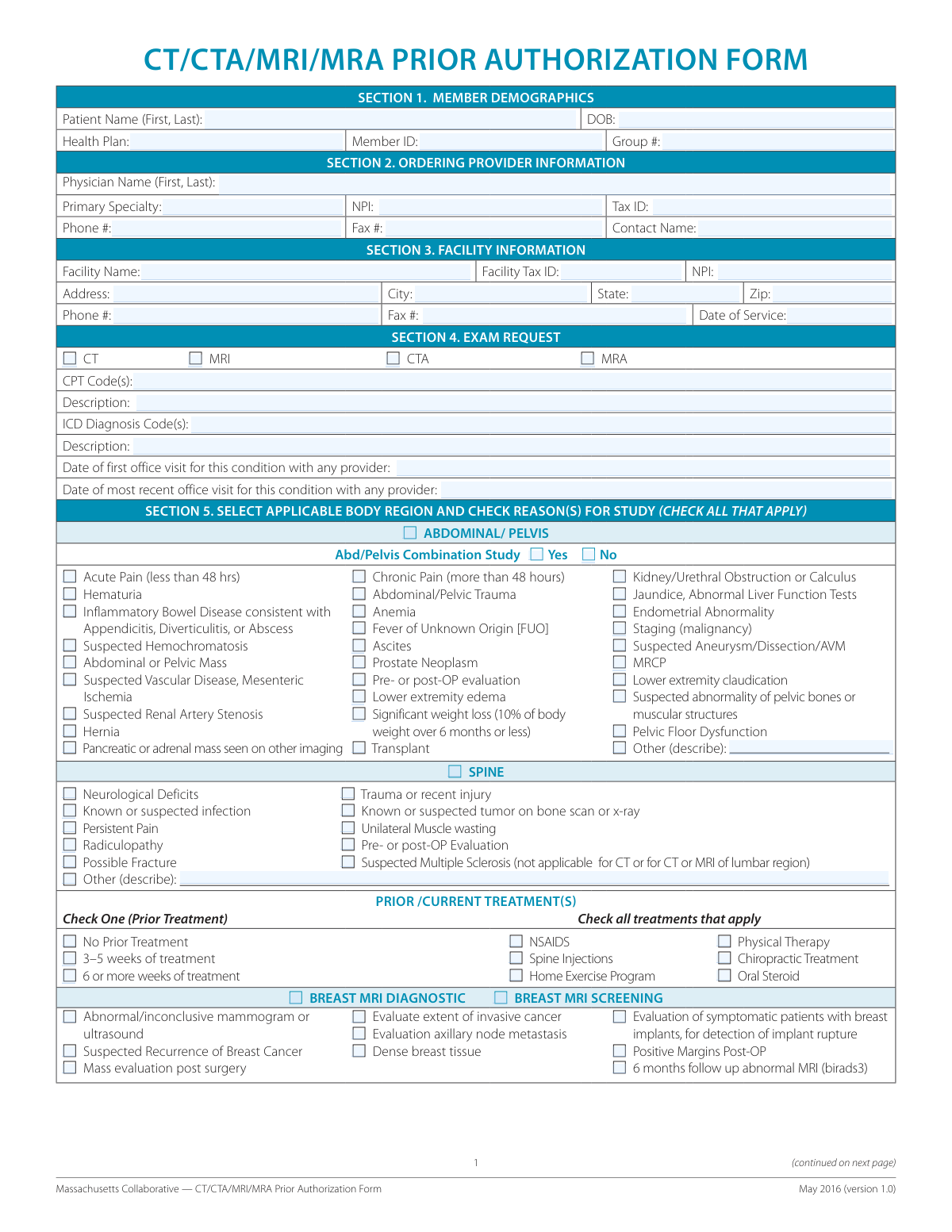
Fill out radiology authorization forms
with AI.
Radiology authorization forms are critical documents in the healthcare industry, serving as the bridge between clinical necessity and insurance coverage. These forms are required before a patient can undergo advanced diagnostic imaging, such as CT scans, MRIs, or PET scans. Their primary purpose is to ensure that the requested procedure is medically appropriate for the patient's condition, which helps prevent unnecessary medical expenses and ensures that healthcare providers receive reimbursement from insurance carriers.
By continuing, you acknowledge Instafill's Privacy Policy and agree to get occasional product update and promotional emails.
About radiology authorization forms
Healthcare providers, including primary care physicians and specialists, typically initiate these forms when they determine that a patient requires detailed imaging to diagnose or monitor a health issue. For example, a doctor in Massachusetts might use a collaborative CT/MRI authorization form, while a provider in Texas might need a specific TMHP request form for Medicaid patients. Without a correctly processed authorization, patients may face significant out-of-pocket costs or delays in their diagnostic journey, making accurate and timely submission essential for both the clinic and the patient.
Managing the paperwork for multiple imaging requests can be a significant administrative burden for busy medical offices. Tools like Instafill.ai use AI to fill these forms in under 30 seconds, handling sensitive data accurately and securely to streamline the pre-approval process. By automating these repetitive tasks, medical staff can focus more on patient care rather than navigating complex PDF fields.
Forms in This Category
- Enterprise-grade security & data encryption
- 99%+ accuracy powered by AI
- 1,000+ forms from all industries
- Complete forms in under 60 seconds
How to Choose the Right Form
Selecting the correct radiology authorization form is essential for ensuring that your patients receive timely care and that your practice avoids claim denials. These forms are primarily categorized by the state in which you practice and the specific insurance program involved.
Choosing by Location and Insurance
The primary differentiator between the forms in this category is the geographical jurisdiction and the payer:
- For Massachusetts Healthcare Providers: If you are requesting advanced imaging services—such as CT, CTA, MRI, or MRA scans—for patients within the state of Massachusetts, you should select the Massachusetts Collaborative — CT/CTA/MRI/MRA Prior Authorization Form. This form is a unified document used by various health plans across the state to streamline the medical necessity review process.
- For Texas Medicaid Providers: If your practice is based in Texas and you are seeking pre-approval for imaging services (including CT, MRI, and PET scans) specifically for Medicaid beneficiaries, use the Radiology Prior Authorization Request Form (Form F00078). This document is required by the Texas Medicaid & Healthcare Partnership (TMHP) to verify that the procedure meets state-mandated medical necessity guidelines.
Why Proper Selection Matters
Using the wrong form can lead to administrative delays, postponed diagnostic procedures, and potential billing issues for the patient. Both the Massachusetts and Texas forms require detailed clinical documentation to justify the imaging request.
Before submitting, ensure you have the patient's clinical history, relevant ICD-10 codes, and previous treatment results ready. Using Instafill.ai, you can quickly complete these complex PDFs by leveraging AI to input patient data accurately, ensuring all required fields for the Massachusetts Collaborative or the Texas TMHP (F00078) forms are addressed before submission.
Form Comparison
| Form | Geographic Focus | Target Payer or Program | Imaging Services Covered |
|---|---|---|---|
| Massachusetts Collaborative — CT/CTA/MRI/MRA Prior Authorization Form | Healthcare providers operating within the state of Massachusetts | Various collaborative health plans and private insurance companies | Advanced imaging including CT, CTA, MRI, and MRA studies |
| Radiology Prior Authorization Request Form | Healthcare providers treating patients within the state of Texas | Texas Medicaid and the Texas Medicaid & Healthcare Partnership | High-tech radiology such as CT, MRI, and PET scans |
Tips for radiology authorization forms
Before filling out a radiology authorization form, ensure you have the patient’s recent clinical notes and previous test results available. Insurance providers require specific evidence of medical necessity to approve advanced imaging like MRIs or CT scans, and having this data ready prevents mid-form delays.
Using outdated or incorrect procedure (CPT) and diagnosis (ICD-10) codes is a frequent cause of authorization denials. Cross-reference your codes with the latest medical billing standards to ensure the form accurately reflects the requested imaging and the patient's condition.
AI-powered tools like Instafill.ai can complete these complex radiology forms in under 30 seconds with high accuracy. Your sensitive data stays secure during the process, providing a reliable and practical time-saving solution for healthcare providers dealing with high volumes of paperwork.
Always double-check the National Provider Identifier (NPI) and tax identification numbers for both the ordering physician and the imaging facility. Missing or incorrect provider details are common administrative errors that can lead to immediate rejection of the authorization request.
Radiology authorizations are typically valid for a specific window, such as 30 to 60 days. Keep a dedicated log of your submitted forms to ensure the imaging procedure is scheduled and performed before the authorization expires to avoid the need for a full resubmission.
Before submitting a prior authorization request, verify that the patient’s insurance policy is active and covers the specific imaging modality requested. Submitting forms for terminated policies or uncovered services is a common mistake that causes unnecessary administrative overhead for your clinic.
Frequently Asked Questions
A radiology authorization form is used by healthcare providers to request pre-approval from an insurance company before performing advanced imaging tests like MRIs, CT scans, or PET scans. This process ensures that the insurer agrees the procedure is medically necessary and will cover the costs of the service. Without this approval, the claim may be denied, potentially leaving the patient or the provider responsible for the bill.
Typically, the office of the referring physician—the doctor who orders the imaging—is responsible for completing and submitting the authorization form. They possess the clinical notes and medical history required to justify the need for the scan. While the radiology facility may assist in tracking the status, the clinical data must come from the ordering provider.
Providers in Massachusetts often use the Massachusetts Collaborative CT/CTA/MRI/MRA Prior Authorization Form. This standardized document is accepted by many health plans across the state to streamline the request process for advanced diagnostic imaging. Using this collaborative form helps ensure that all necessary clinical information is captured in a format familiar to local insurers.
For patients covered under Texas Medicaid, providers must use Form F00078, the Radiology Prior Authorization Request Form. This document is submitted to the Texas Medicaid & Healthcare Partnership (TMHP) for review. It is essential to provide specific clinical indicators required by the state to ensure the procedure is eligible for reimbursement.
Most radiology authorization forms require the patient's diagnosis code (ICD-10), a description of the symptoms, and a history of previous treatments or failed conservative therapies. You may also need to provide results from prior imaging or laboratory tests that support the need for the requested scan. Detailed clinical justification is the most important factor in receiving a timely approval.
The timeline for approval varies by insurance carrier and the urgency of the request, ranging from a few hours to several business days. Routine requests generally take longer, while urgent requests may be processed more quickly if the provider indicates a medical necessity for expedited review. Submitting a complete form with all required clinical documentation helps prevent delays.
Yes, you can use AI tools like Instafill.ai to fill out radiology authorization forms quickly and accurately. These tools can extract relevant data from your clinical notes or patient records and place it directly into the correct fields on the PDF. This method helps reduce manual data entry errors and ensures that all required sections are addressed.
While manually filling out detailed medical forms can take 10 to 15 minutes, AI-powered services can complete the process in under 30 seconds. Tools like Instafill.ai are designed to map data from source documents to the specific requirements of forms like the Texas Medicaid F00078 or the Massachusetts Collaborative form. This significantly speeds up the administrative workflow for busy medical offices.
If a scan is performed before the authorization is secured, the insurance provider will likely deny the claim for the service. In many cases, the provider cannot bill the patient for the balance if the failure to obtain authorization was an administrative error. This makes it critical to receive a confirmed authorization number before the patient arrives for their appointment.
No, these forms vary significantly depending on the state and the specific insurance plan. Some states have adopted universal or collaborative forms to simplify the process for providers, while others require unique forms for their specific Medicaid or state-funded programs. Always verify which form is required by the patient's specific health plan before submission.
Glossary
- Prior Authorization
- A requirement from a health insurance provider that a physician must obtain approval before a specific medical service, such as a radiology scan, is performed for it to be covered.
- Medical Necessity
- The clinical justification provided by a healthcare professional to prove that a requested imaging test is essential for diagnosing or treating a patient's specific medical condition.
- CT / CTA
- Computed Tomography (CT) uses X-rays to create cross-sectional images of the body, while Computed Tomography Angiography (CTA) specifically focuses on visualizing blood vessels.
- MRI / MRA
- Magnetic Resonance Imaging (MRI) uses magnetic fields to produce detailed images of organs and tissues, while Magnetic Resonance Angiography (MRA) specifically examines the blood vessels.
- CPT Code
- Current Procedural Terminology codes are five-digit numbers used to identify the specific medical or diagnostic procedure being requested for billing and authorization purposes.
- ICD-10 Code
- A standardized system of codes used by healthcare providers to classify and report specific diagnoses and symptoms on authorization forms.
- TMHP
- The Texas Medicaid & Healthcare Partnership is the group responsible for processing claims and managing prior authorizations for patients enrolled in Texas Medicaid programs.
- PET Scan
- Positron Emission Tomography is an advanced imaging test that uses a radioactive tracer to show how tissues and organs are functioning at a cellular level.