Fill out Cigna forms
with AI.
Cigna forms are essential documents used by healthcare providers and patients to navigate the complexities of health insurance coverage. These forms serve as the primary communication channel between medical practices and the insurer, ensuring that treatments, medications, and referrals are properly documented and approved. Managing these documents accurately is critical for securing coverage, preventing claim denials, and ensuring that patients receive the care they need without facing unexpected financial burdens.
By continuing, you acknowledge Instafill's Privacy Policy and agree to get occasional product update and promotional emails.
About Cigna forms
Typically, these forms are handled by medical billing staff, office administrators, or physicians who need to request pre-approval for specific services. For instance, Prior Authorization forms are required before administering certain treatments or prescribing non-formulary medications to prove medical necessity. Similarly, Referral Disclosure forms are used when a patient needs to see an out-of-network specialist, ensuring all parties understand the potential costs involved. Navigating these requirements is a daily task for healthcare clinics aiming to maintain smooth operations and high patient satisfaction.
Completing these detailed documents manually can be a significant administrative burden, often leading to delays in patient care. Tools like Instafill.ai use AI to fill these forms in under 30 seconds, handling data accurately and securely to streamline the entire submission process. This allows healthcare professionals to focus more on patient outcomes rather than repetitive paperwork.
Forms in This Category
| Form Name | Pages | |
|---|---|---|
| 1. | Cigna Medication Prior Authorization Form | 2 |
| 2. | Cigna Out-of-Network Referral Disclosure Form | 2 |
| 3. | Cigna Prior Authorization Form | 2 |
- Enterprise-grade security & data encryption
- 99%+ accuracy powered by AI
- 1,000+ forms from all industries
- Complete forms in under 60 seconds
How to Choose the Right Form
Navigating insurance requirements is essential for ensuring that medical treatments are covered and that patients avoid unexpected out-of-pocket costs. To select the right Cigna document, you must first identify whether your request concerns a general medical service, a specific prescription, or a specialist referral.
Medical Procedures and Services
If you are a healthcare provider planning a surgery, diagnostic test, or specialized therapy for a patient, use the Cigna Prior Authorization Form. This document is required to confirm that the proposed medical service is considered medically necessary under the patient’s specific plan. Submitting this form before rendering services helps confirm coverage and prevents claim denials after the fact.
Prescription Medications
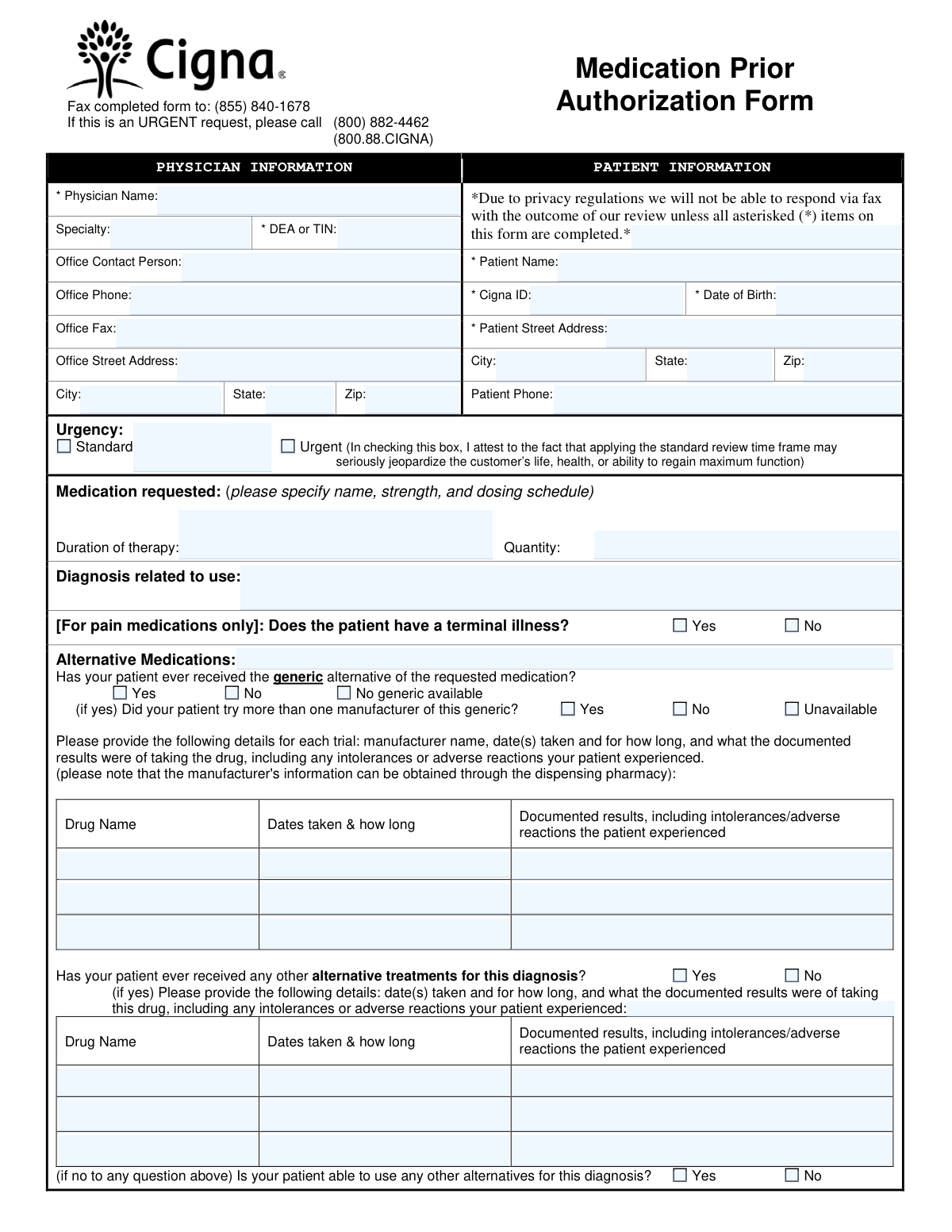
When a patient requires a drug that is not on Cigna's standard preferred list (formulary) or requires special clinical oversight, you must submit the Cigna Medication Prior Authorization Form. This form allows physicians to document medical necessity and list previous treatment attempts to justify the use of a specific medication. It is the primary tool for securing coverage for non-preferred or specialty drugs.
Referrals to Non-Participating Providers
If you are referring a patient to a specialist or facility that is not part of the Cigna provider network, the Cigna Out-of-Network Referral Disclosure Form is mandatory. This form is designed to protect both the provider and the patient by:
- Informing the patient that they may face higher out-of-pocket costs for out-of-network care.
- Documenting that the patient was offered an in-network alternative but chose to proceed with a non-participating provider.
- Disclosing any financial interest the referring physician may have in the out-of-network facility.
Using Instafill.ai simplifies this process by converting these often complex PDF versions into interactive, fillable forms, ensuring that healthcare offices can submit accurate documentation to Cigna quickly.
Form Comparison
| Form | Primary Use | Service Type | Key Goal |
|---|---|---|---|
| Cigna Medication Prior Authorization Form | Requesting coverage for non-preferred or restricted prescription medications. | Prescription drugs and pharmacy benefits. | Demonstrate medical necessity to ensure insurer payment for drugs. |
| Cigna Out-of-Network Referral Disclosure Form | Disclosing potential out-of-pocket costs for using non-network providers. | Out-of-network medical facilities or specialists. | Ensure patient informed consent regarding financial liability and alternatives. |
| Cigna Prior Authorization Form | Obtaining pre-approval for specific medical procedures or clinical services. | Surgeries, hospitalizations, and specialized medical treatments. | Confirm clinical necessity and plan coverage before service delivery. |
Tips for Cigna forms
To avoid delays with prior authorizations, attach relevant clinical notes or lab results that prove medical necessity. Cigna often requires evidence that alternative treatments were tried first before approving non-preferred medications or procedures.
Incorrect insurance ID or NPI numbers are the most common reasons for form rejection. Always cross-reference the patient's Cigna ID card and the physician's credentials before submitting to ensure the data matches the insurer's records.
When referring patients to non-participating providers, ensure the patient signs the disclosure form before the appointment. This protects both the provider and the patient by documenting informed consent regarding potential out-of-pocket costs.
Processing times for medical and medication authorizations can vary based on the complexity of the request. Aim to submit these forms at least three to five business days before the scheduled service to ensure approval is in place.
AI-powered tools like Instafill.ai can complete complex Cigna forms in under 30 seconds with high accuracy. Your data stays secure during the process, making it a reliable practical time-saver for healthcare offices handling multiple authorizations daily.
Always save a copy of the completed PDF and any confirmation numbers received during the submission process. Having a clear digital trail is essential if you need to file an appeal or follow up on a pending request later.
Frequently Asked Questions
Cigna forms are essential documents used to manage healthcare benefits, request pre-approvals for treatments, and document referrals to specialists. These forms help ensure that medical services and prescriptions are covered under a patient's specific insurance plan before costs are incurred. Using the correct form is necessary for both providers and patients to facilitate smooth claims processing and financial transparency.
In most cases, the healthcare provider or physician is responsible for completing and submitting the prior authorization form to Cigna. They must provide clinical documentation to demonstrate that a proposed procedure or medication is medically necessary for the patient's condition. Patients should follow up with their doctor's office to ensure the request has been initiated and approved before receiving treatment.
This form is required when a prescribed drug is not on Cigna's standard preferred drug list or requires specific clinical oversight. It allows your doctor to explain why a specific medication is necessary, especially if you have already tried other covered alternatives without success. Without an approved authorization, the insurance company may not cover the cost of the prescription at the pharmacy.
This form is used when a Cigna-participating physician refers a patient to a provider or facility that is not part of the Cigna network. It serves as a formal notice to the patient that they may face higher out-of-pocket costs by going out-of-network. The form ensures the patient is aware of in-network alternatives and has consented to the potential financial implications of the referral.
Yes, you can use AI-powered tools like Instafill.ai to complete Cigna forms efficiently. These tools can extract relevant data from your existing medical records or source documents and populate the form fields automatically, often in under 30 seconds. This technology helps reduce manual entry errors and ensures that all required sections are completed accurately.
While manual entry can take 15 to 20 minutes depending on the complexity of the medical data, using an AI service can significantly shorten the process. AI tools can analyze your documentation and fill the form in less than a minute. This allows healthcare administrators and patients to spend less time on paperwork and more time on actual care.
Most forms require the patient's member ID, date of birth, and contact information, along with the provider's NPI number and tax ID. Additionally, you will need to provide specific ICD-10 diagnosis codes and CPT procedure codes related to the requested service. Detailed clinical notes or a history of previous treatments are often attached to support the request.
The correct form depends on whether you are requesting a specific medication, a medical procedure, or a referral to a non-participating provider. If you are a healthcare provider, you should select the form that matches the service category—medication-specific forms for prescriptions and general prior authorization forms for surgeries or diagnostic tests. Patients should consult their provider or Cigna's member portal if they are unsure which document is required.
Once submitted, Cigna's clinical review team evaluates the request against their medical necessity guidelines and the patient's specific plan benefits. The provider and patient are typically notified of the decision—approval, denial, or a request for more information—via mail or an online portal. If approved, an authorization number is issued, which must be included when the final claim is submitted for payment.
Requirements vary depending on whether the plan is an HMO, PPO, or Open Access plan. While most plans require prior authorization for major procedures and specialty drugs, some plans may have more flexible referral requirements. It is always best to check the specific summary of benefits for your plan to confirm which forms are mandatory before seeking specialized care.
Glossary
- Prior Authorization (PA)
- A requirement by Cigna that your healthcare provider must obtain approval before certain services or medications are covered by your insurance plan.
- Medical Necessity
- The criteria used by Cigna to determine if a service or medication is essential and appropriate for a patient's specific health condition.
- Out-of-Network (OON)
- Healthcare providers or facilities that do not have a contract with Cigna, which often results in higher out-of-pocket costs for the patient.
- Formulary
- A list of prescription drugs covered by Cigna, which may be categorized into tiers that determine the patient's share of the cost.
- Step Therapy
- A process where Cigna requires a patient to try one or more cost-effective medications for a condition before they will authorize a more expensive drug.
- NPI (National Provider Identifier)
- A unique 10-digit identification number issued to healthcare providers in the United States, required on Cigna forms for processing.
- ICD-10 Code
- A standardized system of diagnostic codes used by medical professionals to classify health conditions on insurance and authorization forms.
- Disclosure
- A formal statement on a form that informs the patient of their financial responsibilities or a physician's interest when being referred to an out-of-network provider.