Fill out medical credentialing forms
with AI.
Medical credentialing forms and provider enrollment documents are the backbone of the healthcare administration process. These forms ensure that healthcare professionals and facilities meet the rigorous standards required by insurance networks and regulatory bodies. Completing these applications accurately is essential for providers to receive reimbursement for services, maintain legal compliance, and establish trust with patients and insurance carriers alike.
By continuing, you acknowledge Instafill's Privacy Policy and agree to get occasional product update and promotional emails.
About medical credentialing forms
This category primarily serves healthcare administrators, private practice owners, and medical groups who are navigating the complex process of joining provider networks or updating their facility information. Whether you are submitting a Provider Group/Facility Application (RA-02) for a specific insurance network or managing a large roster of practitioners, these forms require meticulous attention to detail regarding licensing, NPI numbers, and specialized certifications. Because these documents are often lengthy and repetitive, managing them manually can lead to administrative bottlenecks and delays in provider onboarding.
To streamline this administrative burden, tools like Instafill.ai use AI to fill these forms in under 30 seconds while ensuring data is handled accurately and securely. This allows medical staff to focus more on patient care and less on the repetitive task of data entry across multiple enrollment documents.
Forms in This Category
| Form Name | Pages | |
|---|---|---|
| 1. | Provider Group/Facility Application (RA-02) | 1 |
- Enterprise-grade security & data encryption
- 99%+ accuracy powered by AI
- 1,000+ forms from all industries
- Complete forms in under 60 seconds
How to Choose the Right Form
Navigating medical credentialing and provider enrollment can be a complex process, as each insurance carrier and state health department requires specific documentation to verify the qualifications of healthcare providers. Choosing the correct form ensures that your facility or group practice can begin billing and seeing patients under a specific network without administrative delays.
Enrollment for Organizations and Groups
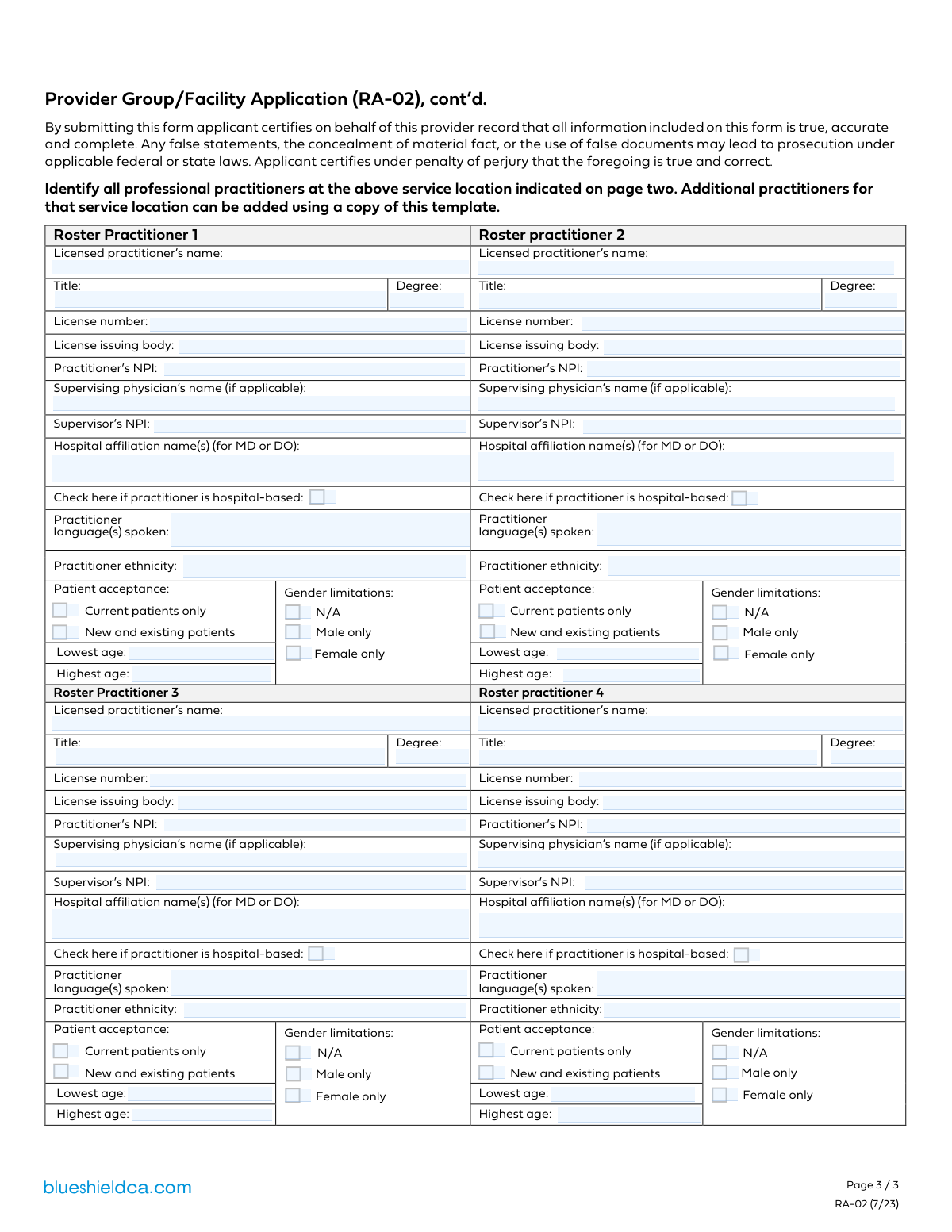
If you are representing a medical group, clinic, or healthcare facility looking to join the Blue Shield of California network, the primary document you will need is the Provider Group/Facility Application (RA-02). This form is specifically designed for organizational enrollment rather than individual solo practitioners who may be filing independently.
You should select the Provider Group/Facility Application (RA-02) if:
- You are establishing a new group contract or updating an existing one with Blue Shield of California.
- You need to provide a comprehensive roster of all professional practitioners working within your facility.
- You are reporting organizational details such as NPI numbers, tax IDs, and specialization categories for a collective group of providers.
Preparing Your Credentialing Data
Before you begin filling out your forms on Instafill.ai, ensure you have the following data ready to ensure accuracy and speed:
- Organizational Data: Legal business name, Tax ID (TIN), and Type 2 NPI.
- Practitioner Roster: A complete list of all doctors, nurses, and specialists, including their individual Type 1 NPIs and current state licenses.
- Operational Policies: Specific details regarding patient acceptance policies and languages spoken within the facility.
Streamlining the RA-02 Process
The Provider Group/Facility Application (RA-02) is often a lengthy document with numerous fields for practitioner data. Using Instafill.ai allows you to convert this complex PDF into an interactive, fillable format. Our AI tools help you map your existing organizational data directly into the form, ensuring that every required field—from specialization codes to licensing details—is completed accurately before you submit it to the carrier.
Form Comparison
| Form | Organization Type | Primary Purpose | Key Requirements |
|---|---|---|---|
| Provider Group/Facility Application (RA-02) | Medical groups and healthcare facilities seeking network participation. | Applying for inclusion in the Blue Shield of California provider network. | Organization details, practitioner roster, NPI numbers, and licensing information. |
Tips for medical credentialing forms
Ensure every practitioner's National Provider Identifier (NPI) and state license number matches official records exactly. Even a single digit error can lead to a rejected application and cause significant delays in the credentialing and enrollment process.
When filling out group applications like the RA-02, ensure your list of practitioners includes current specializations and accurate patient acceptance statuses. Providing outdated information regarding which providers are accepting new patients can result in network directory inaccuracies and compliance issues.
AI-powered tools like Instafill.ai can complete complex medical credentialing forms in under 30 seconds with high accuracy. This technology ensures your sensitive data stays secure during the process while significantly reducing the administrative burden of repetitive data entry.
Many insurance payers cross-reference group applications with individual CAQH ProView profiles. Before submitting your facility forms, ensure all provider data is synchronized between your internal records and the CAQH database to avoid data discrepancies that trigger manual reviews.
If a section does not apply to your facility, use 'N/A' rather than leaving the field blank. Unmarked fields often trigger automated systems to flag the application as incomplete, which pauses the enrollment timeline until you provide written clarification.
Credentialing forms often require attachments such as W-9 forms, proof of professional liability insurance, and accreditation certificates. Having these digital files ready to upload alongside your application will streamline the entire submission process and prevent last-minute searching for critical paperwork.
Frequently Asked Questions
Medical credentialing forms are used by insurance networks and healthcare organizations to verify the qualifications, experience, and professional standing of practitioners and facilities. Completing these forms is a critical step for providers who wish to participate in a specific health plan's network and receive reimbursement for services.
These forms are typically completed by solo practitioners, medical groups, or administrative staff at healthcare facilities like hospitals and clinics. Any entity seeking to join an insurance panel or update their existing contract information must submit these documents to the respective payer.
You will generally need your National Provider Identifier (NPI), state medical licenses, DEA certifications, board certifications, and professional liability insurance details. For group applications, you will also need a comprehensive roster of all practitioners associated with the organization's tax identification number.
A group application focuses on the business entity and its collective roster of practitioners rather than a single doctor. It establishes the billing relationship for the entire facility and ensures that all associated providers meet the network's quality standards.
Yes, AI tools like Instafill.ai can fill these forms in under 30 seconds by accurately extracting and placing data from your source documents into the PDF. This process eliminates manual data entry and helps ensure that complex fields are populated correctly based on your professional records.
While manual completion can take hours due to the volume of data required, using an AI-powered service can reduce that time to less than a minute. These platforms can also convert non-fillable PDF versions into interactive forms, making the entire submission process more efficient.
While initial enrollment is the most intensive phase, most insurance networks require re-credentialing every two to three years to maintain active status. Additionally, you must submit update forms whenever there is a change in practice location, tax ID, or the list of practitioners working within a group.
Completed forms are usually submitted directly to the provider relations or credentialing department of the specific insurance carrier, such as Blue Shield of California. Many payers now allow for digital submission via their secure provider portals or through email as specified in the application instructions.
Incomplete applications are often pended or rejected, which can significantly delay your ability to bill for services and see in-network patients. Using automated tools can help ensure that all required fields are addressed by identifying missing data points before you finalize the document.
Yes, the National Provider Identifier is a standard requirement for almost all healthcare administrative transactions in the United States. Both individual providers (Type 1) and organizations (Type 2) must provide their specific NPI to be correctly identified in the payer's system.
Many credentialing forms serve a dual purpose of enrolling new groups or updating the practitioner roster for existing ones. This ensures the insurance network has an up-to-date list of which doctors are currently seeing patients and are authorized to bill under the group's contract.
Glossary
- NPI (National Provider Identifier)
- A unique 10-digit identification number issued to healthcare providers in the United States by the Centers for Medicare & Medicaid Services (CMS).
- Credentialing
- The formal process of verifying a healthcare provider's education, training, experience, and professional license to ensure they meet the standards for providing care.
- Provider Enrollment
- The administrative process of applying to a health insurance network so that a medical provider or facility can bill the insurer for services rendered to members.
- Practitioner Roster
- A comprehensive list of all healthcare professionals working within a group or facility, typically including their individual specialties, license numbers, and NPIs.
- TIN (Tax Identification Number)
- A nine-digit number used by the IRS to identify a business entity, which is required on credentialing forms to link the medical group to its tax and payment records.
- Board Certification
- A voluntary designation that indicates a physician has reached a high level of expertise in a specific medical specialty through additional training and testing.
- Privileging
- The process where a healthcare organization authorizes a practitioner to perform specific clinical services or procedures based on their verified credentials and performance.
- CAQH ProView
- An industry-standard online database where providers upload their professional information to be shared with multiple health plans for credentialing purposes.