Fill out precertification forms
with AI.
Precertification forms, often referred to as prior authorization or pre-authorization documents, are essential tools in the healthcare industry used to verify that a proposed medical service, treatment, or procedure is medically necessary before it is performed. These forms serve as a vital communication link between healthcare providers and insurance companies, ensuring that the costs associated with specialized care—such as advanced radiology, cardiology, or behavioral health services—will be covered under a patient's specific plan. Completing these forms correctly is a critical step in preventing claim denials and ensuring that patients receive necessary care without unexpected financial complications.
By continuing, you acknowledge Instafill's Privacy Policy and agree to get occasional product update and promotional emails.
About precertification forms
Typically, these forms are completed by physicians, clinical staff, or medical billing specialists. They are required in a wide range of scenarios, from requesting supplemental information for an existing claim to authorizing specialized treatments like Applied Behavior Analysis (ABA). Because these documents require precise clinical findings, CPT codes, and treatment rationales, the manual entry process can be labor-intensive and susceptible to errors. Tools like Instafill.ai use AI to fill these precertification forms in under 30 seconds, handling sensitive data accurately and securely to help providers save valuable administrative time.
Forms in This Category
- Enterprise-grade security & data encryption
- 99%+ accuracy powered by AI
- 1,000+ forms from all industries
- Complete forms in under 60 seconds
How to Choose the Right Form
Choosing the Correct Precertification Form
Navigating insurance requirements is essential to ensure medical services are covered and claims are not denied. Precertification forms are primarily used by healthcare providers to demonstrate medical necessity before a procedure occurs. To select the right document, identify whether you are initiating a new request or responding to a request for more information.
Behavioral Health and ABA Therapy
If you are a provider seeking authorization for Applied Behavior Analysis (ABA) therapy for patients diagnosed with Autism Spectrum Disorder, you must use the Outpatient Behavioral Health (BH) – ABA Treatment Request (GR-69017-4). This is a specialized form for Aetna and its affiliates (including Innovation Health and Banner | Aetna). It is designed to capture specific CPT codes and treatment hours required for behavioral health reviews.
Advanced Imaging and Cardiac Procedures
For high-tech diagnostic services, select the Precertification request form: Advanced Radiology and Cardiology Services. This form is the standard starting point for securing approval for complex imaging (like MRIs or CT scans) and heart-related procedures. Using this form ensures the insurance carrier reviews the clinical necessity before the patient arrives for their appointment.
Supplemental Data for Existing Requests
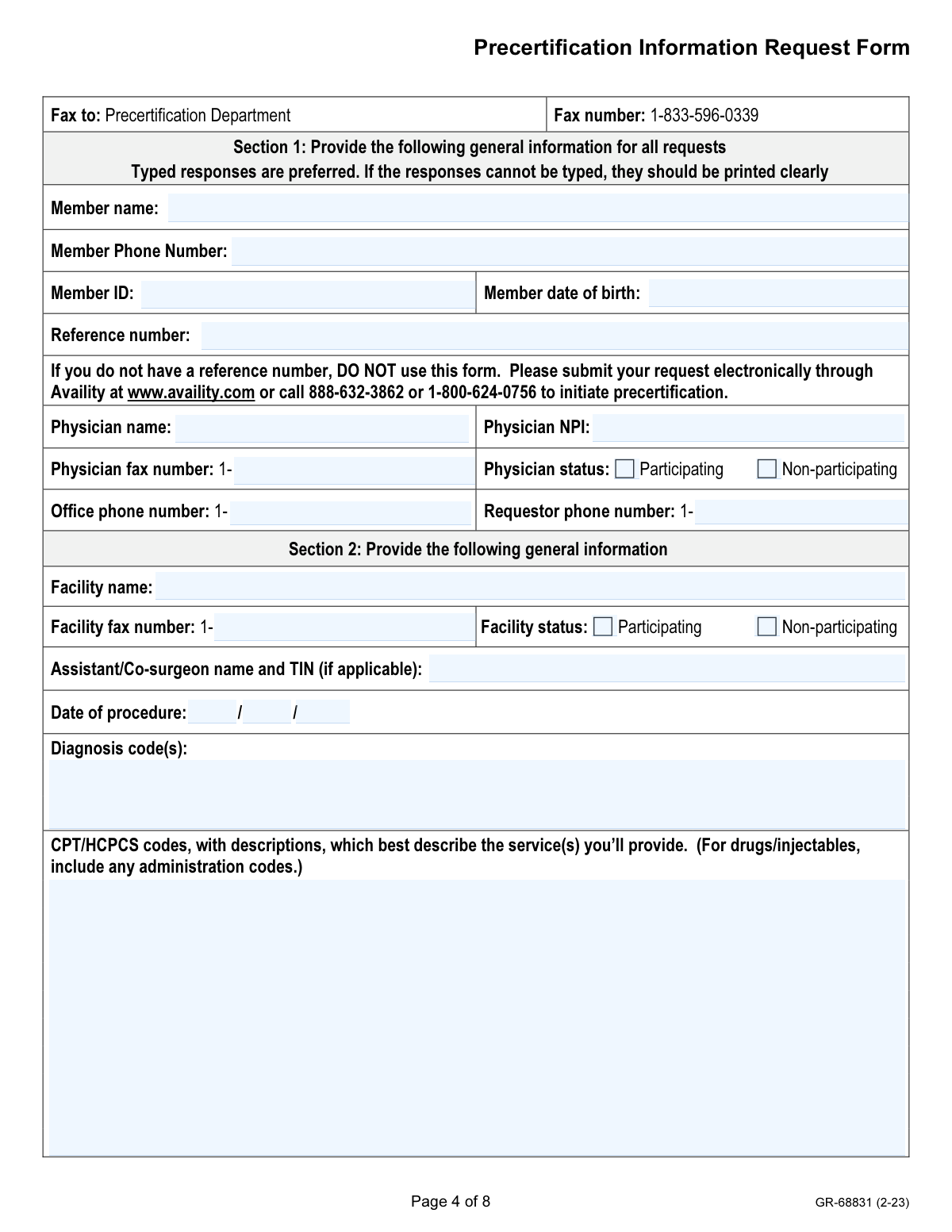
If you have already submitted a precertification request and the insurance company has asked for more clinical evidence, do not start a new application. Instead, use Form GR-68831, Precertification Information Request Form. This document is specifically designed to provide supplemental medical history, clinical findings, and treatment rationale for a request that is already in the system, helping to prevent delays in the approval process.
Quick Selection Tips
- Starting a new ABA therapy plan? Use GR-69017-4.
- Scheduling an MRI or Stress Test? Use the Advanced Radiology and Cardiology form.
- Adding notes to a pending Aetna case? Use Form GR-68831.
Form Comparison
| Form | Medical Focus | Primary Purpose | Timing of Submission |
|---|---|---|---|
| Form GR-68831, Precertification Information Request Form | General medical supplemental information | Provides additional clinical findings for an existing request | After a precertification request has already been initiated |
| Outpatient Behavioral Health (BH) – ABA Treatment Request: Required Information for Precertification (GR-69017-4) | Behavioral Health and ABA therapy | Requests authorization for Applied Behavior Analysis for Autism | Before outpatient ABA treatment services are rendered |
| Precertification request form: Advanced Radiology and Cardiology Services | Radiology and Cardiology procedures | Ensures advanced imaging and heart services are covered | Prior to performing advanced radiology or cardiology services |
Tips for precertification forms
Ensure the procedure codes (CPT) and diagnosis codes (ICD-10) on the precertification form match your clinical documentation exactly. Discrepancies between the form and the patient’s medical chart are a leading cause of processing delays or immediate administrative denials.
Some forms, such as the Aetna GR-68831, are specifically designed to provide supplemental information for an existing request rather than starting a new one. Always verify if you are initiating a new authorization or responding to a request for additional clinical evidence to ensure the correct workflow is followed.
AI-powered tools like Instafill.ai can complete complex precertification forms in under 30 seconds with high accuracy, even when dealing with multi-section behavioral health or cardiology documents. Your data stays secure during the process, providing a practical and reliable way to handle high volumes of insurance paperwork.
For specialized services like ABA therapy or advanced radiology, ensuring the supervising provider's NPI and credentials are correct is vital for reimbursement. Incorrect provider data can cause a form to be rejected before the clinical review even begins, delaying essential patient care.
Most precertification requests require supporting documentation such as recent office notes, lab results, or previous imaging reports. Ensure these attachments are clearly labeled and directly support the medical necessity of the requested service to help the insurance reviewer reach a decision faster.
Insurance carriers frequently update their precertification requirements and form versions, such as the transition to new ABA treatment request forms. Always check that you are using the most current version of the form to avoid rejection due to outdated documentation standards.
Frequently Asked Questions
A precertification form is a document submitted by a healthcare provider to an insurance company to verify that a proposed medical service is covered and medically necessary. Obtaining this approval before the procedure is performed helps ensure that the insurance company will pay for the service according to the member's plan benefits.
Typically, the healthcare provider, such as a physician or a specialized clinic, is responsible for filling out and submitting precertification forms. While the provider handles the clinical details, patients should monitor the process to ensure approval is received before their scheduled appointment to avoid unexpected costs.
Form GR-68831 is specifically used as a supplemental document to provide additional clinical information for a request that has already been initiated. It is not intended to start a new precertification process but rather to offer deeper clinical findings or treatment rationale requested by the insurer.
For outpatient ABA therapy services under Aetna and its affiliate plans, you must use Form GR-69017-4. This form is mandatory for members diagnosed with Autism Spectrum Disorder and requires detailed information regarding CPT codes, treatment hours, and provider credentials.
If a required precertification is not obtained, the insurance company may deny the claim entirely or apply a financial penalty. This often results in the patient being responsible for a larger portion of the bill or the provider's claim being rejected for lack of prior authorization.
Yes, AI tools like Instafill.ai can be used to fill out these forms by accurately extracting data from source documents and placing it into the correct fields. This technology allows providers to complete complex medical forms in under 30 seconds, significantly reducing administrative overhead.
While manual entry for detailed medical forms can take 15 to 20 minutes, using an AI-powered service like Instafill.ai can complete the process in under 30 seconds. The AI handles data extraction and form population automatically, ensuring that even non-fillable PDFs become interactive and easy to complete.
Precertification forms often require accompanying clinical evidence such as physician progress notes, diagnostic test results, and treatment history. For specialized services like radiology or cardiology, you may also need to include specific imaging reports that justify the necessity of the requested advanced procedure.
No, precertification forms are generally specific to the insurance carrier or the healthcare network administering the plan. For instance, the GR-series forms are specific to Aetna and its partners, so you must ensure you are using the document designated by the patient's specific insurance provider.
Completed forms are usually submitted to the insurance company's utilization management or prior authorization department via a secure online portal, fax, or mail. The specific submission instructions, including the correct fax number or web address, are typically found on the form itself or the insurer's provider website.
Glossary
- Precertification
- The process of obtaining approval from a health insurance company before a specific medical service, treatment, or procedure is performed to ensure it is covered under the patient's plan.
- Medical Necessity
- A standard used by insurers to determine if a service is appropriate and required for the diagnosis or treatment of a patient's condition based on established clinical guidelines.
- CPT Code
- Current Procedural Terminology; a standardized set of five-digit codes used by healthcare providers to identify the specific medical services and procedures being requested for authorization.
- ABA (Applied Behavior Analysis)
- A specialized therapy used primarily for individuals with Autism Spectrum Disorder that requires detailed clinical documentation and specific precertification forms for insurance approval.
- Advanced Radiology
- High-tech diagnostic imaging procedures, such as MRI, CT, and PET scans, which typically require a more rigorous precertification process than standard X-rays.
- Clinical Rationale
- The medical reasoning and evidence provided by a physician to explain why a specific treatment or diagnostic test is necessary for a patient's health outcomes.
- Attending Provider
- The primary healthcare professional responsible for a patient's care who is required to complete and sign the precertification request forms.
- Behavioral Health (BH)
- A category of medical care encompassing mental health and substance abuse services that often involves unique authorization requirements for outpatient treatment.