Fill out CareSource forms
with AI.
CareSource forms cover a range of administrative and clinical documents that providers, members, and caregivers need to navigate healthcare services within the CareSource network. This category focuses on forms used to request approvals, document medical necessity, and coordinate care — particularly for specialized services that require prior authorization before treatment can begin. These forms play a critical role in ensuring that members receive appropriate, covered care while helping providers meet compliance and billing requirements.
By continuing, you acknowledge Instafill's Privacy Policy and agree to get occasional product update and promotional emails.
About CareSource forms
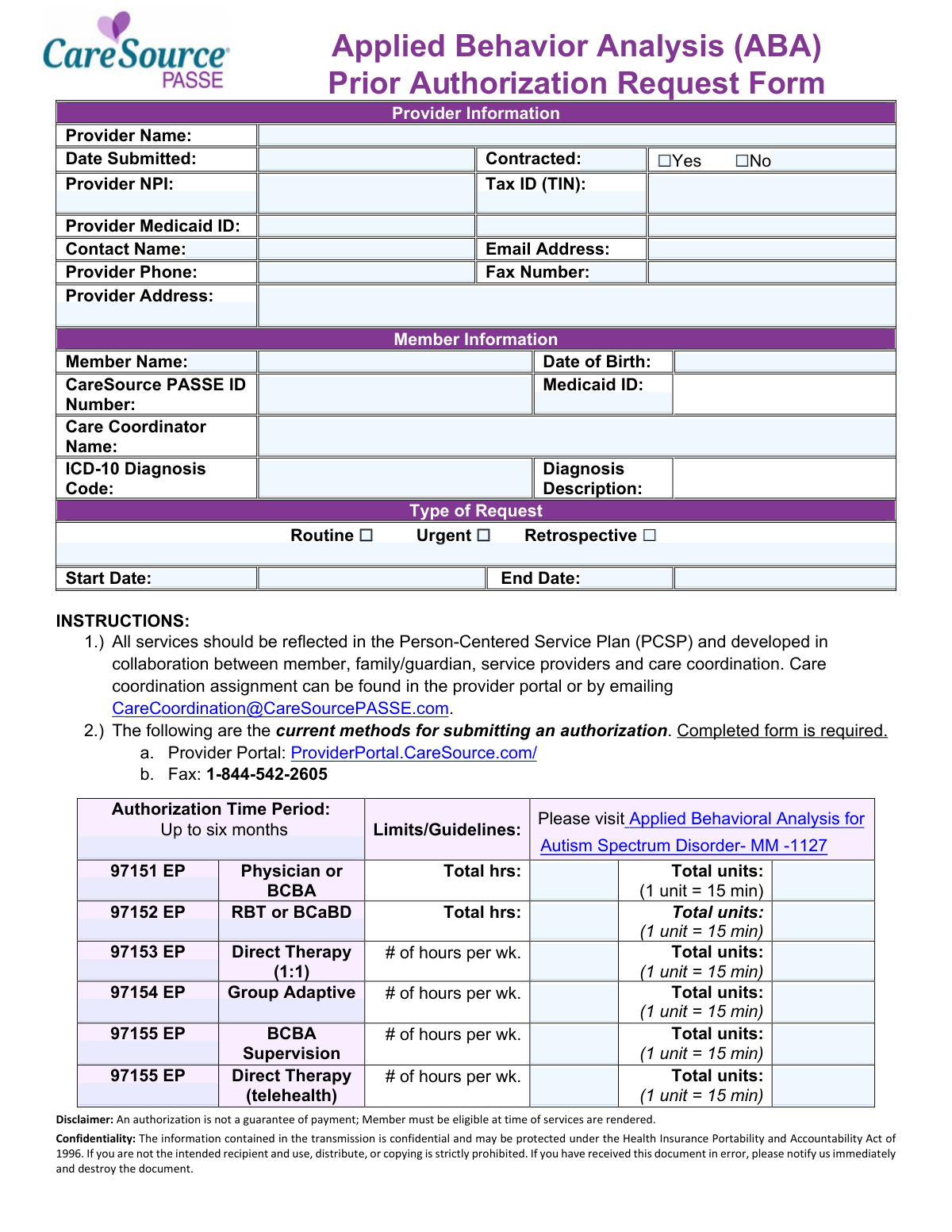
The forms in this category are most commonly used by healthcare providers — including behavioral health specialists, therapists, and clinical supervisors — who need to obtain pre-approval for services delivered to CareSource members. For example, the Applied Behavior Analysis (ABA) Prior Authorization Request Form is essential for providers seeking approval to deliver ABA therapy to members diagnosed with Autism Spectrum Disorder, covering everything from direct therapy sessions to parent training and BCBA supervision. Timely and accurate completion of these forms directly affects whether services can proceed and whether claims will be reimbursed.
Because prior authorization forms require precise clinical and administrative details — diagnosis codes, service codes, member information, and supporting documentation — errors or omissions can cause costly delays. Tools like Instafill.ai use AI to fill these forms in under 30 seconds, helping providers submit accurate, complete requests without the usual administrative burden.
Forms in This Category
| Form Name | Pages | |
|---|---|---|
| 1. | CareSource PASSE Applied Behavior Analysis (ABA) Prior Authorization Request Form | 2 |
- Enterprise-grade security & data encryption
- 99%+ accuracy powered by AI
- 1,000+ forms from all industries
- Complete forms in under 60 seconds
How to Choose the Right Form
With only one form currently available in this category, choosing the right one is straightforward — but knowing *when* and *why* to use it is just as important.
ABA Therapy Prior Authorization
The CareSource PASSE Applied Behavior Analysis (ABA) Prior Authorization Request Form is the form you need if:
- You are a provider or BCBA seeking pre-approval to deliver ABA therapy services to a CareSource PASSE member
- Your patient has a confirmed Autism Spectrum Disorder (ASD) diagnosis and requires services such as direct therapy, BCBA supervision, parent/family training, or group adaptive behavior sessions
- You are billing under service codes 97151–97158 EP and need authorization before rendering services
Who Should Complete This Form
This form is intended for healthcare providers and BCBAs, not members or families. If you are a caregiver seeking services for a loved one, contact your provider or CareSource PASSE directly to initiate the process.
Before You Submit
Make sure you have the following ready:
- Member and provider information (NPI, member ID, contact details)
- Diagnosis codes supporting the ASD determination
- Requested service codes, hours, and units
- A copy of the member's Person-Centered Service Plan (PCSP)
Important Reminders
- Authorization is not a guarantee of payment — member eligibility must be confirmed at the time services are rendered
- Incomplete submissions can delay approval, so double-check all fields before submitting
- If you're working with a non-fillable PDF version of this form, tools like Instafill.ai can convert it into an interactive, AI-assisted fillable form to speed up completion and reduce errors
Form Comparison
| Form | Purpose | Who Files It | When to Use |
|---|---|---|---|
| CareSource PASSE Applied Behavior Analysis (ABA) Prior Authorization Request Form | Request pre-approval for ABA therapy services for autism members | Healthcare providers and BCBAs serving CareSource PASSE members | Before delivering ABA therapy, supervision, or family training services |
Tips for CareSource forms
Always confirm that the member is actively enrolled in CareSource PASSE coverage before submitting a prior authorization request. Authorization approval does not guarantee payment if the member is found ineligible at the time services are actually rendered, so eligibility checks should be a routine first step.
The ABA Prior Authorization form requires specific CPT service codes ranging from 97151 to 97158 EP — using incorrect or outdated codes is one of the most common reasons for delays or denials. Double-check that each requested service type (direct therapy, BCBA supervision, parent training, group sessions) is matched to its correct corresponding code before submission.
Incomplete submissions are a leading cause of authorization delays. Include the member's Autism Spectrum Disorder diagnosis documentation, the Person-Centered Service Plan (PCSP), and any assessments or clinical notes required to justify the requested hours and units at the time of initial submission.
Vague or miscalculated hour and unit requests can trigger additional review or outright denial. Calculate the exact number of units needed for each service type based on the member's treatment plan, and ensure the totals are consistent across all sections of the form.
AI-powered tools like Instafill.ai can fill out the CareSource PASSE ABA Prior Authorization form with high accuracy in under 30 seconds, reducing manual entry errors and saving significant time — especially valuable when managing authorizations for multiple members. Your data stays secure throughout the process, making it a practical solution for busy provider offices.
Always save a dated copy of the completed form and any confirmation of submission for your records. If a payment dispute arises later, having documented proof of your prior authorization request — including submission date and attached supporting materials — can be critical.
A common misconception is that receiving an authorization approval means payment is secured. CareSource PASSE authorization only confirms the service plan was pre-approved; actual payment depends on member eligibility at the time of service, correct billing, and adherence to the approved plan.
Frequently Asked Questions
This form is used by providers to request pre-approval from CareSource PASSE before delivering Applied Behavior Analysis (ABA) therapy services to members diagnosed with Autism Spectrum Disorder. It covers services such as direct therapy, BCBA supervision, parent/family training, and group adaptive behavior sessions. Submitting this form is a required step before services can be rendered and billed.
Healthcare and behavioral health providers — including BCBAs and ABA therapy practices — who treat CareSource PASSE members and require pre-approval for specific services must complete these forms. The forms are not typically filled out by members or patients themselves. Providers are responsible for ensuring the form is complete and submitted on time.
Providers should submit the prior authorization request before delivering ABA therapy services, as authorization must be in place prior to rendering care. Submitting the form as early as possible helps avoid delays in treatment and ensures the member is eligible at the time services begin. Late or incomplete submissions can result in non-payment even if services were provided.
The form requires provider details, member information, Autism Spectrum Disorder diagnosis codes, applicable service codes (such as 97151–97158 EP), requested hours and units, and supporting clinical documentation. It also needs to align with the member's Person-Centered Service Plan (PCSP). Having all this information ready before starting the form will speed up the process significantly.
No — authorization is not a guarantee of payment. Members must be eligible under their CareSource PASSE plan at the time services are actually rendered. Providers should verify member eligibility both before submitting the authorization request and before each service date.
Completed forms are typically submitted directly to CareSource PASSE through their designated submission channels, which may include fax, an online provider portal, or mail. Providers should refer to their CareSource PASSE provider agreement or the contact information on the form itself for the most current submission instructions.
Yes — AI-powered tools like Instafill.ai can fill out CareSource prior authorization forms in under 30 seconds by accurately extracting and placing data from source documents such as clinical records or provider profiles. This reduces manual entry errors and speeds up the submission process. Instafill.ai can also convert non-fillable PDF versions of these forms into interactive, fillable formats.
Manually completing the form can take 15–30 minutes depending on how readily available the required clinical and member information is. Using an AI-assisted tool like Instafill.ai, the form can be populated in under 30 seconds by automatically extracting relevant data from uploaded source documents. This is especially helpful for practices handling multiple authorization requests at once.
The form covers ABA therapy service codes ranging from 97151 to 97158 EP, which correspond to various types of ABA assessments, direct therapy, supervision, and group adaptive behavior treatment. Providers should ensure they are requesting authorization for the specific codes that match the services planned for the member. Using incorrect codes can result in denial or delay of authorization.
Yes — CareSource PASSE (Provider-led Arkansas Shared Savings Entity) is a managed care program specific to Arkansas, designed to serve Medicaid members with complex needs including developmental disabilities. This prior authorization form is intended for providers operating within the CareSource PASSE network in Arkansas. Providers outside this network should check with their respective CareSource plan for applicable forms.
An incomplete form or missing supporting documentation can result in delays, requests for additional information, or outright denial of the authorization request. It is important that providers include all required clinical documentation and ensure the requested services align with the member's Person-Centered Service Plan. Double-checking the form before submission helps avoid unnecessary back-and-forth with CareSource PASSE.
Glossary
- Prior Authorization (PA)
- Advance approval required from CareSource before a provider can deliver certain services or treatments to a member. Without prior authorization, payment for the service may be denied even if the service is medically necessary.
- PASSE
- Provider-led Arkansas Shared Savings Entity — a managed care organization in Arkansas that coordinates physical, behavioral, and developmental health services for Medicaid members with complex needs, including those with Autism Spectrum Disorder.
- Applied Behavior Analysis (ABA)
- A structured, evidence-based therapy used primarily to improve social, communication, and learning skills in individuals diagnosed with Autism Spectrum Disorder (ASD). ABA services require prior authorization from CareSource PASSE before they can be billed.
- BCBA (Board Certified Behavior Analyst)
- A credentialed professional who designs, supervises, and oversees ABA therapy programs. On CareSource forms, BCBA supervision hours must be separately identified and authorized.
- Service Codes (97151–97158 EP)
- Standardized CPT billing codes used to identify specific ABA therapy services, such as assessments, direct treatment, and group adaptive behavior sessions. Each code corresponds to a distinct service type that must be individually authorized on the form.
- Person-Centered Service Plan (PCSP)
- An individualized care plan developed collaboratively with the member and their support team that outlines their goals, needs, and approved services. ABA therapy hours requested must align with the member's PCSP to be considered for authorization.
- Autism Spectrum Disorder (ASD)
- A developmental condition affecting communication, behavior, and social interaction, and the primary qualifying diagnosis required for ABA therapy authorization through CareSource PASSE.
- Units
- The standard measurement used to quantify ABA therapy services for billing and authorization purposes, typically representing 15-minute increments of service time. Providers must specify the number of units requested for each service code on the form.
- Rendering Provider
- The individual clinician or therapist who directly delivers the ABA therapy services to the member, as distinct from the billing provider or supervising BCBA. The rendering provider's NPI and credentials must be included on the authorization form.
- NPI (National Provider Identifier)
- A unique 10-digit identification number assigned to healthcare providers by the federal government, required on CareSource authorization forms to identify both the billing organization and the individual rendering provider.