Fill out MetroPlusHealth forms
with AI.
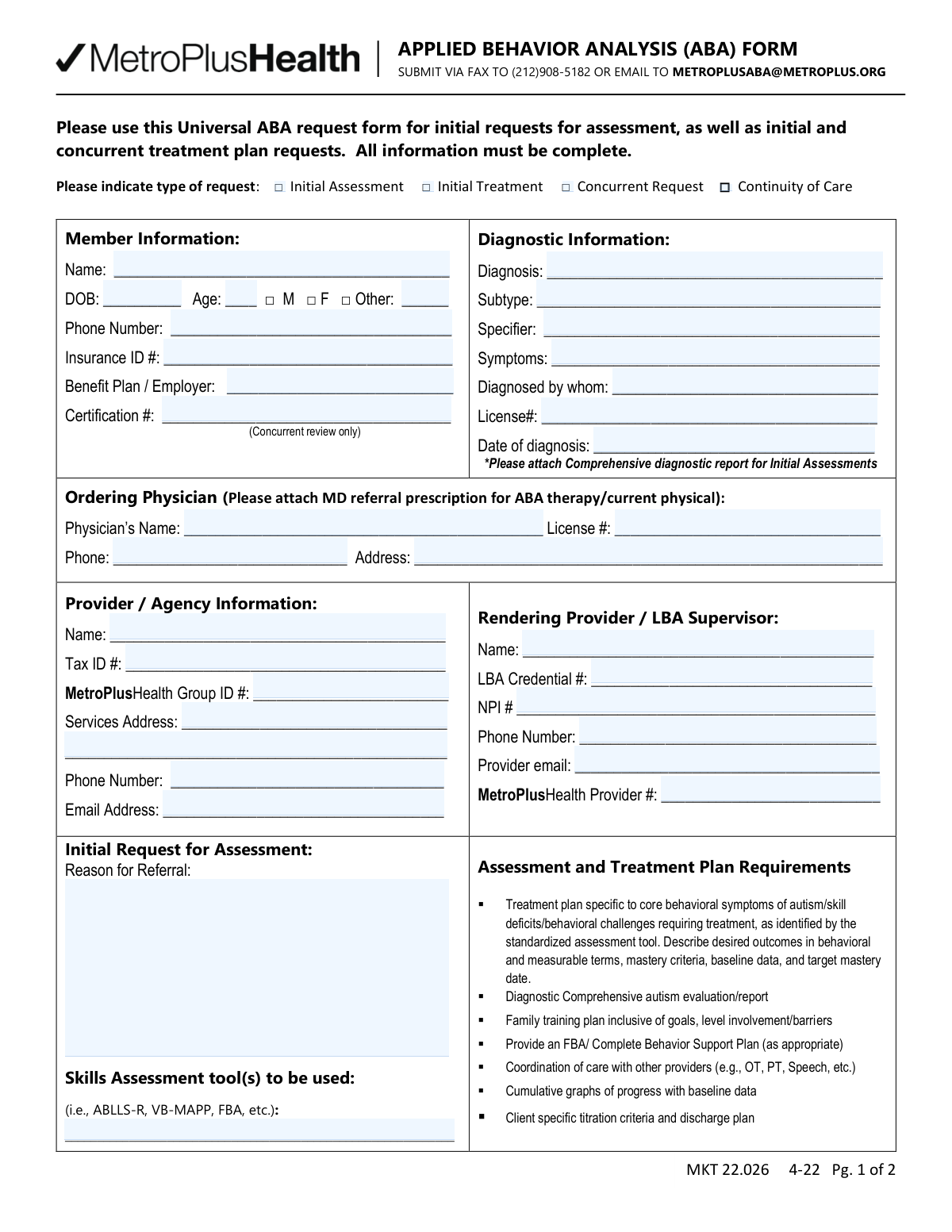
MetroPlusHealth forms cover a range of administrative and clinical documents used by healthcare providers, agencies, and members to coordinate care, request authorizations, and meet plan requirements. These forms play a critical role in ensuring that services are approved and delivered without unnecessary delays — particularly for specialized care that requires prior authorization or detailed clinical documentation. One key example in this category is the Applied Behavior Analysis (ABA) Universal Request Form, which providers use to submit authorization requests for ABA therapy services on behalf of members, including diagnostic information, treatment plans, and CPT codes.
By continuing, you acknowledge Instafill's Privacy Policy and agree to get occasional product update and promotional emails.
About MetroPlusHealth forms
These forms are typically completed by healthcare providers, behavioral health agencies, and clinical staff who need to initiate or continue services for MetroPlusHealth members. Situations commonly requiring these forms include initial assessments, new treatment plan submissions, concurrent stay reviews, and continuity of care requests. Accurate and complete submission is essential — missing information or incorrect coding can result in delays or outright denials of medically necessary services.
For providers managing multiple cases, tools like Instafill.ai use AI to fill these forms in under 30 seconds, handling the data accurately and securely, which can make a meaningful difference in day-to-day administrative workload.
Forms in This Category
| Form Name | Pages | |
|---|---|---|
| 1. | MetroPlusHealth Applied Behavior Analysis (ABA) Universal ABA Request Form | 2 |
- Enterprise-grade security & data encryption
- 99%+ accuracy powered by AI
- 1,000+ forms from all industries
- Complete forms in under 60 seconds
How to Choose the Right Form
Navigating healthcare authorizations can be complex, but MetroPlusHealth simplifies the process for Applied Behavior Analysis (ABA) services by utilizing a consolidated document for most clinical requests. Currently, the primary document available in this category is the MetroPlusHealth Applied Behavior Analysis (ABA) Universal ABA Request Form.
When to Use This Form
This form is the standard requirement for healthcare providers and agencies seeking payer authorization for ABA services for MetroPlusHealth members. You should select this form if you are managing any of the following clinical stages:
- Initial Assessment Requests: Use this when a member first requires a diagnostic evaluation to determine the medical necessity of ABA therapy.
- Initial Treatment Plans: Select this option once the assessment is complete and you are proposing a specific clinical intervention strategy for a new patient.
- Concurrent/Continued Stay Reviews: This is necessary for existing patients who require ongoing therapy beyond their current authorization window to prevent a lapse in service.
- Continuity of Care: Use this for members transitioning from another provider or insurance plan who need to maintain their current treatment schedule without interruption.
Essential Information for a Successful Submission
To avoid delays or denials, the MetroPlusHealth Applied Behavior Analysis (ABA) Universal ABA Request Form requires specific data points that must be filled out accurately. Before you begin, ensure you have the following information ready:
- Provider and Member Details: Full identification for the rendering agency and the MetroPlusHealth member.
- Service Specifications: You must clearly define the requested CPT codes, the specific units per week, and the designated place of service.
- Clinical Justification: The form requires diagnostic information and details regarding the ordering physician.
- Required Attachments: Be prepared to include comprehensive diagnostic reports and updated treatment plan elements as part of your submission.
Using Instafill.ai to complete this form allows you to turn the standard PDF into a streamlined, fillable document, ensuring that all technical codes and member data are entered precisely to meet medical necessity criteria.
Form Comparison
| Form | Primary Purpose | Required Documentation | Filing Frequency |
|---|---|---|---|
| MetroPlusHealth Applied Behavior Analysis (ABA) Universal ABA Request Form | Requesting authorization for ABA services, including initial assessments and continued treatment plans. | Diagnostic reports, ordering physician details, treatment plan elements, and specific CPT codes. | Submitted for initial assessments, treatment plan updates, or concurrent stay reviews. |
Tips for MetroPlusHealth forms
Always double-check that the member's name and identification number match the details on their MetroPlusHealth insurance card exactly. Small discrepancies in spelling or ID digits can lead to immediate administrative denials or significant processing delays.
MetroPlusHealth requires specific supporting documents, such as comprehensive diagnostic reports and updated treatment plans, to justify medical necessity. Failing to attach these files when submitting your request will often result in the form being returned for more information.
Clearly list the CPT codes and the requested units per week for each service type to ensure proper authorization. Miscalculating units or using outdated codes can cause issues during the billing and reimbursement phase after services are rendered.
AI-powered tools like Instafill.ai can complete these complex healthcare forms in under 30 seconds with high accuracy. Your data stays secure during the process, making it a reliable and practical time-saver for providers dealing with multiple authorization requests.
Ensure the NPI and contact information for the ordering physician are accurate and legible on the form. This information is critical for MetroPlusHealth to verify that the ABA services were professionally recommended according to plan requirements.
Distinguish clearly between an initial assessment, a first-time treatment plan, or a concurrent stay review. Selecting the wrong request type can trigger the wrong review workflow, potentially delaying the start of care for the member.
Verify that the Place of Service indicated on the form aligns with where the ABA therapy will actually occur, whether in-home or at a clinic. Misalignment between the service location and the requested codes can lead to authorization errors.
Frequently Asked Questions
MetroPlusHealth forms are primarily used by healthcare providers and agencies to request prior authorization for specialized medical or behavioral services. These documents ensure that the requested treatment, such as Applied Behavior Analysis (ABA), meets the health plan's medical necessity criteria and is covered under the member's specific plan.
The form is typically completed by the healthcare provider or the behavioral health agency providing the services. While the form requires member details, the clinical information, CPT codes, and diagnostic data must be provided by the ordering physician or the lead BCBA to ensure clinical accuracy.
Yes, you can fill out MetroPlusHealth forms using AI technology. AI tools like Instafill.ai can fill these forms in under 30 seconds, accurately extracting and placing data from your source documents directly into the required PDF fields.
Manually filling out complex behavioral health forms can be time-consuming due to the level of clinical detail required. However, using an AI-powered service like Instafill.ai allows you to complete the entire form in less than 30 seconds by automating the data entry process.
Most MetroPlusHealth ABA requests must be accompanied by a comprehensive diagnostic report and a detailed treatment plan. These attachments provide the clinical justification for the requested units and help the utilization management team review the case for approval.
Completed forms are generally submitted to the MetroPlusHealth Behavioral Health or Utilization Management department via a secure provider portal or a designated fax number. Always check the footer or the header of the specific form for the most up-to-date submission instructions.
An initial assessment request is for members who have not yet started ABA services with your agency, while a concurrent or continued stay review is for members already receiving care who need additional units. The Universal ABA Request Form allows you to select the appropriate request type at the top of the document.
Submitting an incomplete form often leads to administrative delays or an immediate denial of the request. It is vital to ensure that all mandatory fields, such as the member's ID number, CPT codes, and the ordering physician's signature, are clearly filled out before submission.
These forms are generally used for members enrolled in MetroPlusHealth Medicaid Managed Care, Child Health Plus, and certain Marketplace plans. Providers should always verify the member's eligibility and specific benefit package before submitting an authorization request.
The form is designed to cover a range of ABA-related services, including initial clinical assessments, direct 1-on-1 therapy, and supervision. Providers must specify the exact CPT codes and the number of units requested per week for each specific service category.
Glossary
- Applied Behavior Analysis (ABA)
- A type of therapy that focuses on improving specific behaviors, such as social skills, communication, and reading, often used for individuals with autism or other developmental disorders.
- Prior Authorization
- The process by which a healthcare provider obtains approval from MetroPlusHealth before providing a service to ensure the treatment is covered under the member's plan.
- CPT Codes
- Current Procedural Terminology codes are a standardized set of numbers used to identify the specific medical, surgical, or diagnostic services being requested for billing and tracking.
- Medical Necessity
- The criteria used by health plans to determine if a requested service or treatment is reasonable, necessary, and appropriate for the patient's specific diagnosis.
- Concurrent Review
- An ongoing evaluation of a member's treatment plan while they are receiving care to determine if continued services are still medically necessary.
- Continuity of Care
- A process that allows a member to continue receiving services from a specific provider for a limited time during a transition between health plans or providers.
- Units of Service
- The specific quantity of therapy requested, often measured in 15-minute increments or hourly blocks per week, depending on the CPT code used.
- Ordering Physician
- The licensed medical doctor who provides the formal diagnosis and signs the referral or request for ABA services.