Fill out insurance claim forms
with AI.
Insurance claim forms are the official documents required to request benefits or reimbursement from an insurance provider after a qualifying medical event, illness, disability, or hospitalization. Whether you're filing a critical illness claim with an Aflac Group insurer like CAIC, submitting a disability claim through Prudential or Assurity Life, or seeking pre-authorization for cashless hospitalization, these forms serve as the formal record that insurers use to verify eligibility, assess medical necessity, and calculate the benefits owed to you. Completing them accurately — with the right diagnoses, procedure codes, physician signatures, and supporting documentation — is essential to avoiding delays, denials, or requests for resubmission.
By continuing, you acknowledge Instafill's Privacy Policy and agree to get occasional product update and promotional emails.
About insurance claim forms
These forms are used by a wide range of people: patients recovering from serious illness, employees on medical leave filing disability claims, healthcare providers billing insurers for professional services, and family members navigating claims on behalf of a loved one. Some forms, like the CMS-1500, are completed by medical billing staff, while others, such as attending physician statements or employment history questionnaires, require input from multiple parties before submission.
Because these forms often involve dense medical terminology, precise coding requirements, and strict formatting rules, errors are common when filling them out manually. Tools like Instafill.ai use AI to fill these forms in under 30 seconds, handling the data accurately and securely — a practical time-saver whether you're managing a single claim or processing multiple forms at once.
Forms in This Category
- Enterprise-grade security & data encryption
- 99%+ accuracy powered by AI
- 1,000+ forms from all industries
- Complete forms in under 60 seconds
How to Choose the Right Form
Start by identifying who is filing and what type of claim you need to submit — the forms here serve very different purposes.
Critical Illness Claims (Aflac/CAIC)
- If you have a Continental American Insurance Company (CAIC) or Aflac Group policy and were diagnosed with a qualifying critical illness, use the CAIC / Aflac Group Critical Illness Claim Form. This is a complete packet that includes the physician's statement, HIPAA authorization, and optional direct deposit setup — submit it all together.
Disability Insurance Claims
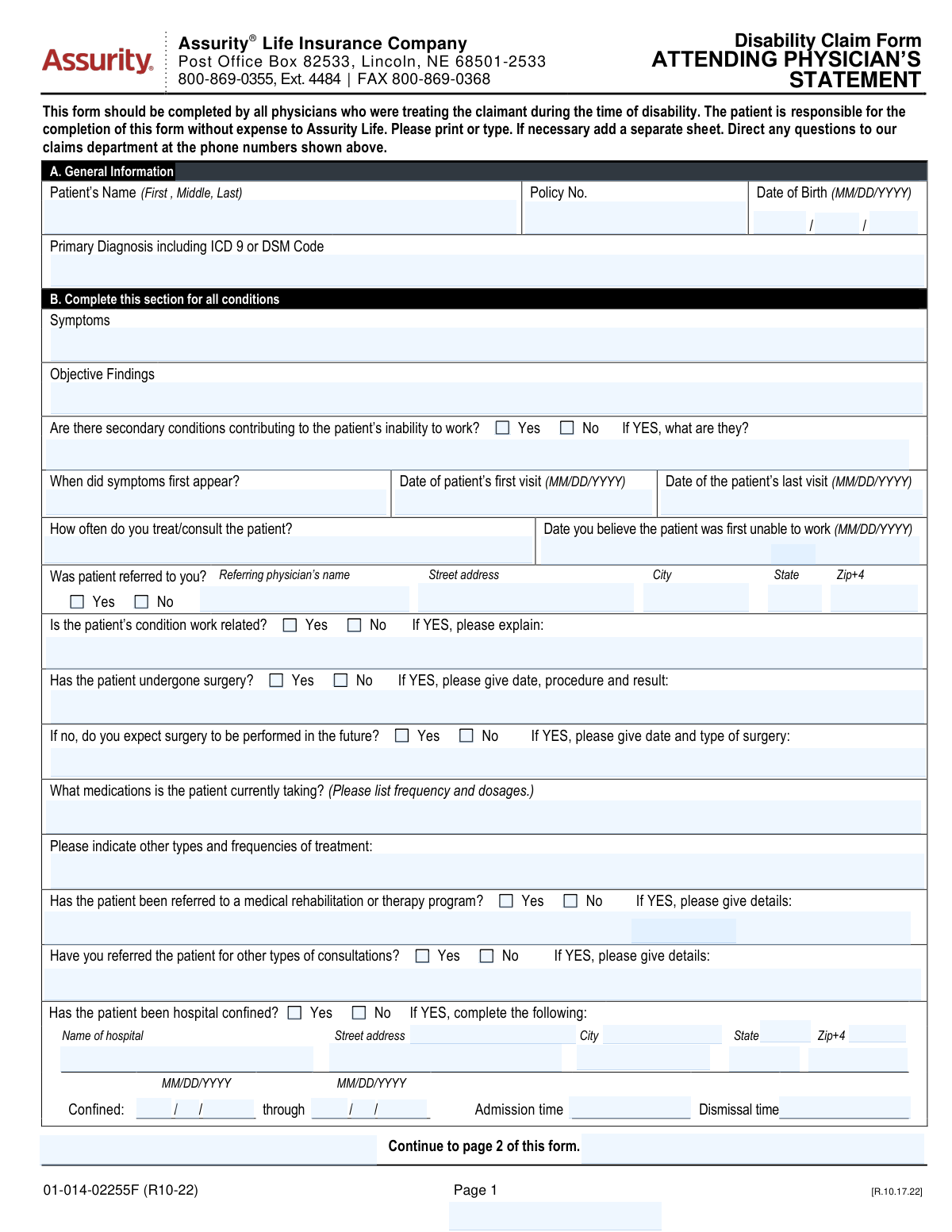
- Physicians completing a medical statement for a disabled patient covered by Assurity Life should use the Assurity Life Insurance Company Disability Claim Form – Attending Physician's Statement.
- Prudential claimants documenting their work history and vocational background should use the Prudential Group Disability Insurance – Education and Employment History Form (GL.2009.009). Note: this form appears twice in the list — both versions are the same form, so either will work.
Medical/Health Insurance Claims
- Healthcare providers billing insurers for professional services (doctor visits, outpatient procedures) should use the CMS-1500 (02-12) Health Insurance Claim Form — the standard form accepted by Medicare, Medicaid, and most private payers.
- Patients in India seeking cashless hospitalization through an HDFC ERGO policy should use the HDFC ERGO Request for Cashless Hospitalisation (Policy Part – C), which must be submitted to the network hospital before or during admission.
Quick Decision Summary
| Situation | Use This Form |
|---|---|
| Aflac/CAIC critical illness diagnosis | CAIC / Aflac Critical Illness Claim Form |
| Doctor documenting a disability (Assurity) | Assurity Attending Physician's Statement |
| Prudential disability — work/education history | Prudential GL.2009.009 |
| Provider billing a health insurer | CMS-1500 |
| HDFC ERGO cashless hospital treatment | HDFC ERGO Cashless Hospitalisation Form |
If you're unsure which form applies, check your insurance policy documents or contact your insurer directly before filling out any form.
Form Comparison
| Form | Purpose | Who Files It | When to Use |
|---|---|---|---|
| Continental American Insurance Company (CAIC) / Aflac Group Critical Illness Claim Form | File a critical illness insurance benefit claim | Policyholder, patient, and attending physician | After diagnosis of a qualifying critical illness event |
| Assurity Life Insurance Company Disability Claim Form — Attending Physician's Statement | Provide medical evidence supporting a disability claim | Treating/attending physician | When substantiating patient's disability for Assurity insurer |
| The Prudential Insurance Company of America Group Disability Insurance – Education and Employment History Form (GL.2009.009, Ed. 06/2017) | Document work history and skills for disability evaluation | Claimant/disabled employee | During ongoing Prudential group disability claim review |
| CMS-1500 (02-12), Health Insurance Claim Form (NUCC Approved) (OMB 0938-1197) | Submit professional medical claims to health insurers | Healthcare providers and medical billers | When billing payers for outpatient or professional services |
| Prudential Group Disability Insurance – Education and Employment History Form (GL.2009.009, Ed. 06/2017) | Report employment and education background for disability review | Claimant/disabled employee | During Prudential disability claim vocational assessment |
| HDFC ERGO General Insurance Company Limited – Request for Cashless Hospitalisation for Health Insurance (Policy Part – C) | Request pre-authorization for cashless hospital treatment | Insured patient and treating hospital | Before or at admission to a network hospital in India |
Tips for insurance claim forms
Insurance claim forms — especially critical illness and disability claims — require medical records, physician statements, policy numbers, and diagnosis codes. Having these on hand before you begin prevents mid-form delays and reduces the chance of submitting incomplete information that could trigger a denial.
Forms like the CMS-1500 require precise ICD diagnosis codes and CPT/HCPCS procedure codes. Even a single incorrect or outdated code can result in claim rejection, delayed reimbursement, or an audit. Always verify codes against current coding guidelines before submitting.
Many claim packets — including CAIC/Aflac and Assurity disability forms — require a completed Attending Physician's Statement as part of the submission. Physicians are often busy, so request this section as early as possible to avoid holding up your entire claim while waiting for their signature.
AI-powered tools like Instafill.ai can complete insurance claim forms in under 30 seconds with high accuracy, pulling in your information consistently across multiple forms. Your data stays secure throughout the process, making it a practical time-saver when you're managing several claims or complex multi-part packets like the CAIC/Aflac bundle.
Claim packets like the CAIC/Aflac Critical Illness form include multiple components — the claim form, physician statement, HIPAA authorization, and optional direct deposit form. Submitting all sections together in one package prevents processing delays caused by missing attachments.
Disability claim forms from insurers like Prudential ask for detailed employment and education history going back 15–20 years. Incomplete or vague job descriptions can affect how the insurer assesses your transferable skills and occupational eligibility, so take time to describe duties specifically and accurately.
Pre-authorization forms like the HDFC ERGO cashless hospitalization request must typically be submitted before or at the time of admission — not after discharge. Submitting late can result in the claim being processed as a reimbursement instead, requiring you to pay upfront and wait for repayment.
Always save a dated copy of each completed claim form and any supporting documents you attach. If a claim is disputed, delayed, or requires resubmission, having your original submission on record makes the follow-up process significantly faster and protects you in case of discrepancies.
Frequently Asked Questions
This category includes six forms covering a range of insurance claim needs: a CAIC/Aflac Group Critical Illness Claim packet, an Assurity Life disability claim physician statement, two Prudential Group Disability education and employment history forms, the CMS-1500 health insurance claim form, and an HDFC ERGO cashless hospitalization request. Whether you're filing a critical illness, disability, or general health insurance claim, you'll find the relevant form here.
Insurance claim forms are completed by a combination of policyholders, patients, employers, and medical providers depending on the form type. For example, disability claim forms may require input from both the claimant and their attending physician, while health insurance claim forms like the CMS-1500 are usually submitted by healthcare providers on behalf of patients. Understanding who is responsible for each section helps ensure the form is completed correctly and processed without delays.
The right form depends on your insurer, the type of claim, and your role in the process. For example, if you have a critical illness policy through Aflac or CAIC, you'd use their specific claim packet; if you're a healthcare provider billing a health plan, the CMS-1500 is the standard form. Review your insurance policy documents or contact your insurer directly to confirm which form applies to your situation.
Most insurance claim forms require supporting documentation such as medical records, physician statements, diagnosis codes, and proof of treatment or hospitalization. Some forms, like the CAIC/Aflac Critical Illness packet, include a built-in HIPAA authorization so the insurer can obtain records directly. Gathering complete and accurate documentation before submitting your claim helps prevent processing delays and reduces the risk of denial.
Yes — AI-powered tools like Instafill.ai can fill out insurance claim forms in under 30 seconds by accurately extracting and placing data from your source documents. This is especially useful for complex forms like the CMS-1500 or Prudential disability questionnaires, where precision matters. Instafill.ai can also convert non-fillable PDF versions of these forms into interactive, fillable formats.
Manually completing insurance claim forms can take anywhere from 15 minutes to over an hour, depending on the complexity and the amount of information required. Using an AI tool like Instafill.ai, the same forms can be filled out in under 30 seconds by automatically extracting relevant data from uploaded documents and populating the correct fields.
Most insurers require claims to be submitted within a specific timeframe after a qualifying event, such as a diagnosis, hospital admission, or onset of disability. Filing promptly is important because late submissions can result in reduced benefits or denial of the claim. Always check your policy documents or contact your insurer to confirm the exact filing deadline that applies to your coverage.
A cashless hospitalization form, like the HDFC ERGO form in this category, is a pre-authorization request submitted before or at the time of hospital admission at a network facility. It allows the insurer to verify eligibility and approve payment directly to the hospital, so the patient avoids large out-of-pocket costs upfront. A regular reimbursement claim form, by contrast, is submitted after treatment to recover expenses already paid by the patient.
Yes, most disability insurance claim forms include an Attending Physician's Statement section that must be completed and signed by the treating doctor. This medical evidence is critical because insurers use it to verify the diagnosis, assess the severity of the disability, and determine benefit eligibility and duration. Without a properly completed physician statement, claims are often delayed or denied.
The CMS-1500 is a standardized health insurance claim form used by healthcare providers — such as physicians, therapists, and outpatient clinics — to bill professional medical services to insurance payers, including Medicare, Medicaid, and private insurers. It captures patient and provider information, diagnosis codes, procedure codes, and charges. Accurate completion is essential, as errors can trigger claim denials, audits, or reimbursement delays.
Insurers like Prudential use employment and education history to evaluate a claimant's occupational duties, transferable skills, and vocational options as part of the disability determination process. This information helps the insurer assess whether the claimant can perform their own occupation or any other occupation, which directly affects benefit eligibility under the policy terms. Providing complete and accurate details on these forms is important for a fair and thorough review.
Not always, but many insurer-specific claim packets — such as the CAIC/Aflac Critical Illness packet — include a HIPAA authorization as part of the submission package. This authorization allows the insurer to request medical records directly from healthcare providers to substantiate the claim. If your claim packet does not include one, your insurer may send a separate authorization form or request records through another process.
Glossary
- Attending Physician's Statement (APS)
- A form completed by the treating doctor that provides clinical evidence—such as diagnosis, symptoms, treatment history, and work limitations—to medically support an insurance claim. Insurers require this document to verify that a claimed condition meets the policy's eligibility criteria.
- HIPAA Authorization
- A signed consent form that permits an insurance company to request and review your private medical records from healthcare providers. Without this authorization, insurers are legally prohibited from obtaining the records needed to evaluate your claim.
- Critical Illness Benefit
- A lump-sum or scheduled payment made by an insurer when a policyholder is diagnosed with a specific serious condition listed in the policy, such as cancer, heart attack, or stroke. The qualifying diagnoses and payout amounts are defined in the policy contract.
- Cashless Hospitalisation
- A health insurance arrangement where the insurer pays the hospital directly for covered treatment costs, so the patient does not need to pay upfront and seek reimbursement later. It requires pre-authorization approval through the insurer or a Third-Party Administrator (TPA) before or during admission.
- Third-Party Administrator (TPA)
- An organization hired by an insurance company to handle administrative tasks such as processing claims, verifying eligibility, and coordinating cashless hospitalization approvals. The TPA acts as an intermediary between the insured, the hospital, and the insurer.
- NPI (National Provider Identifier)
- A unique 10-digit identification number assigned to healthcare providers in the United States, required on claim forms like the CMS-1500 to identify the billing and rendering provider. Entering an incorrect or missing NPI is a common reason for claim rejection.
- ICD Code
- A standardized alphanumeric code from the International Classification of Diseases used on claim forms to identify a patient's diagnosis or medical condition. Insurers use these codes to determine whether a condition is covered under the policy.
- CPT/HCPCS Code
- Standardized numeric codes used on health insurance claim forms to describe the specific medical procedures, services, or supplies provided to a patient. Payers use these codes alongside ICD diagnosis codes to calculate reimbursement amounts.
- Electronic Funds Transfer (EFT) Authorization
- An optional form included in some claim packets that allows the insurer to deposit benefit payments directly into your bank account instead of mailing a check. Providing accurate routing and account numbers is essential to avoid payment delays.
- Transferable Skills Assessment
- An evaluation used in disability insurance claims to determine whether a claimant's education, work history, and abilities qualify them for other types of employment, which can affect ongoing benefit eligibility. Insurers use employment history forms to gather the data needed for this analysis.